Introductory Remarks
 |
| Video 1: Introduction [High bandwidth] |
The following collection of video presentations has been generated by Professor Robert H. Anderson, using specimens from the Farouk S. Idriss Cardiac Registry at the Children’s Memorial Hospital of Chicago. Rachid Idriss, the son of Farouk Idriss, is the curator of the archive, which was assembled initially by Dr. Idriss, and which has been carefully conserved and expanded over the years by Drs. Constantine Mavroudis and Carl L. Backer. The archive now contains over 2500 cardiac specimens, the best of which have been selected for these video presentations by Prof. Anderson, a frequent visiting anatomist and morphologist at Children’s Memorial Hospital. The videotapes are grouped together by anatomic diagnosis. Within each anatomic diagnosis, there are demonstrations showing the different features of multiple specimens. The tapes have been edited to produce these versions by Gemma Price, from the Great Ormond Street Hospital, London, England. It is our hope that, in the near future, we will collect and edit comparable videotapes showing the diagnostic features and intraoperative morphology of the various lesions.
General Cardiac Morphology
- Attitudinal Orientation [High bandwidth]
- Sequential Segmental Analysis [High bandwidth]
- Right Atrium [High bandwidth]
- Oval Fossa [High bandwidth]
- Triangle of Koch [High bandwidth]
- Left Atrium [High bandwidth]
- Atrioventricular Junctions [High bandwidth]
- Right Ventricle [High bandwidth]
- Left Ventricle [High bandwidth]
- Arterial Trunks [High bandwidth]
- Coronary Arteries [High bandwidth]
- Coronary Veins [High bandwidth]
- Conduction System [High bandwidth]
 |
| Video 2: Normal Specimen [High bandwidth] |
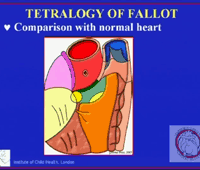 |
| Video 3: Comparing the normal and the ToF heart [High bandwidth] |
Tetralogy of Fallot
In this set of videoclips, we begin with an introduction to the anatomy of the outflow tract of the normal right ventricle, since over the years it has been the rule for morphologists to make comparisons with the building blocks of the normal heart, and the arrangement of these components in the setting of tetralogy of Fallot. The initial videoclip [Video 2], therefore, shows the structure of the right ventricular outflow tract in hearts from a neonate and an adult. These demonstrations of anatomy are then reinforced by reference to a cartoon showing the location of the normal building blocks, a picture of a dissected normal heart, and then a cartoon showing the abnormal location of the building blocks in the setting of tetralogy of Fallot.
We then demonstrate [Video 3] a series of hearts showing the anatomic variability to be found in the setting of tetralogy of Fallot, defined on the basis of subpulmonary obstruction produced in the setting of deviation of the muscular outlet septum, or its fibrous remnant, coupled with an anomalous arrangement of the septoparietal trabeculations, this feature, of course, being combined with biventricular origin of the aorta and an interventricular communication.
In the clip entitled "Tetralogy of Fallot I" [Video 4], we begin with a short review of the normal anatomy as shown in the introductory clips, and follow that with extensive discussion of an example of tetralogy of Fallot with a perimembranous ventricular septal defect, emphasizing the landmarks to the atrioventricular conduction axis.
 |
 |
| Video 4: Tetralogy of Fallot – I [High bandwidth] |
Video 5: Tetralogy of Fallot – II [High bandwidth] |
The next clip, entitled "Tetralogy of Fallot – II" [Video 5], we again show the location of the interventricular communication between the limbs of the septomarginal trabeculation, or septal band. The chosen specimen in this clip, however, shows beautifully the squeeze produced between the deviated outlet septum and the anomalous septoparietal trabeculations, this being the hallmark of the lesion. In this particular specimen, it can also be seen that two-thirds of the circumference of the aortic root is supported within the right ventricle, meaning that the ventriculo-arterial connection is that of double outlet right ventricle, albeit in the setting of tetralogy of Fallot.
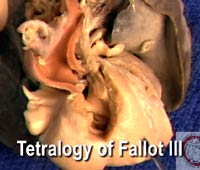 |
| Video 6: Tetralogy of Fallot –III [High bandwidth] |
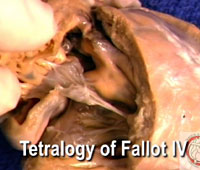 |
| Video 7: Tetralogy of Fallot IV [High bandwidth] |
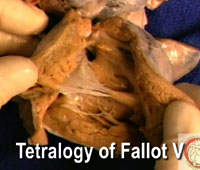 |
| Video 8: Tetralogy of Fallot V [High bandwidth] |
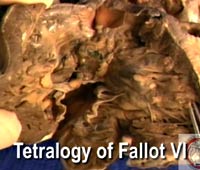 |
| Video 9: Tetralogy of Fallot VI [High bandwidth] |
In the third clip of the series showing the variations in tetralogy (Tetralogy of Fallot – III) [Video 6], we again demonstrate the phenotypic feature of the squeeze between the deviated outlet septum and the anomalous septoparietal trabeculations, but in this specimen with a muscular postero-inferior rim to the interventricular communication. The specimen illustrates well how this muscular rim, which protects the conduction axis, is formed by fusion of the postero-caudal limb of the septomarginal trabeculation with the ventriculo-infundibular fold. The specimen also has a long sub-pulmonary infundibulum, and again has the ventriculo-arterial connection of double outlet right ventricle.
In the fourth clip, entitled "Tetralogy of Fallot – IV" [Video 7], we again show an example with a perimembranous defect, but this time with a much shorted subpulmonary infundibulum, the muscular outlet septum itself being hypoplastic, albeit still deviated in antero-cephalad direction relative to the limbs of the septomarginal trabeculation. The specimen also shows nicely the squeeze between the deviated outlet septum and the hypertrophied septoparietal trabeculations. In this specimen, about half of the aortic valve is supported within the right ventricle, but it is easy to see the fibrous continuity between the leaflets of the aortic and tricuspid valves which makes the defect perimembranous. It is also possible to recognize the remnant of the interventricular component of the membranous septum known as the membranous flap. The specimen is demonstrated so as to show that the crucial border of the interventricular communication is that viewed from the right ventricle.
In the fifth clip [Video 8], the outlet septum is again hypoplastic, as shown also in the second clip showing tetralogy, so that the subpulmonary infundibulum is relatively short. In this specimen, the ventricular septal defect is again perimembranous, the postero-inferior limb of the septomarginal trabeculation stopping short of the ventriculo-infundibular fold. The specimen is then demonstrated so as to show the borders of the interventricular defect as seen from the right ventricle, this being the plane of space defined as the ventricular septal defect. As in the specimen shown in the fourth clip, there is again a membranous flap reinforcing the postero-inferior margin of the defect.
The sixth clip [Video 9] shows a specimen obtained subsequent to attempted surgical repair. A patch had been placed so as to wall the overriding aorta back into the left ventricle, with another patch placed across the ventriculo-pulmonary junction so as to widen the subpulmonary outflow tract. The surgeon had also resected the septoparietal trabeculations, but the stitches securing the patch to the ventricular septum were placed through the septal crest, with haemorrhages suggesting that the sutures had traumatized the atrioventricular conduction axis.
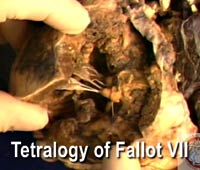
The seventh clip [Video 10] shows another specimen subsequent to attempted surgical repair. The interest in this specimen is the association with straddling and overriding of the tricuspid valve. The specimen shows beautifully the malalignment between the atrial and ventricular septums that is the phenotypic feature of straddling tricuspid valve. The malalignment results in an anomalous origin of the atrioventricular conduction axis, with haemorrhage suggesting that the anomalous conduction tissue was traumatized during the surgical repair.
 |
 |
| Video 10: Tetralogy of Fallot VII [High bandwidth] |
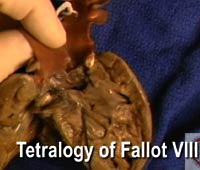
Video 11: Tetralogy of Fallot VIII [High bandwidth] |
The final clip [Video 11] shows us the phenotypic features of tetralogy of Fallot, but with pulmonary atresia rather than pulmonary stenosis. We see nicely the blind-ending subpulmonary infundibulum along with a perimembranous ventricular septal defect. In the specimen shown, the pulmonary arterial supply is derived from the arterial duct.



