Patient Presentation
A 42-year-old man with chronic obstructive pulmonary disease (COPD) presented to the emergency department (ED) complaining of worsening shortness of breath and respiratory distress. His home oxygen requirement was 2 liters by nasal canula, and he has had multiple prior hospital admissions for respiratory failure. His most recent admission was 3 days prior to this presentation, and had required a brief period of endotracheal intubation along with management in the Medical Intensive Care Unit (MICU). He has a past medical history of childhood asthma, polysubstance abuse and hepatitis B and C. He has a 45 pack-year history of smoking, and currently smokes 5-6 cigarettes per day.
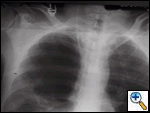 |
| Figure 1. Large right-upper lobe lucency |
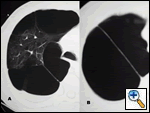 |
| Figure 2. Right hemithorax with smaller bullae |
The patient was afebrile and hemodynamically stable. However, pulse oximetry registered 70% as the patient was receiving 4 liters of oxygen by nasal canula. On physical examination, the patient had diminished breath sounds in the right-upper chest and diffuse expiratory wheezing. An arterial blood gas (ABG) in the ED revealed a pH 7.23, PaCO2 126 mm Hg, PaO2 37 mm Hg and SaO2 72%. An admission chest roentogram was obtained and revealed a large right-upper lobe lucency without evidence of pneumothorax (Figure 1). The patient was endotracheally intubated in the ED for respiratory distress, and a repeat ABG (pH 7.39, PaCO2 83 mm Hg, PaO2 160 mm Hg and SaO2 92%) on ventilator settings of tidal volume 500 ml, no positive end-expiratory pressure, respiratory rate of 20 breaths per minute and 50% FiO2 showed improvement. Following intubation, the patient was admitted to the MICU and aggressive pulmonary therapy was pursued. Intravenous steroids, frequent nebulizers and intravenous antibiotics were also administered. Chest computed tomography (CT) demonstrated a massive right apical bulla occupying nearly one-third of the right hemithorax along with several smaller bullae seen throughout the right and left lungs (Figure 2). The patient subsequently improved, and was able to be extubated on the morning of the second hospital day. A post-extubation ABG on 2 liters of oxygen by nasal canula was pH 7.36, PaCO2 85 mm Hg, PaO2 55 mm Hg and SaO2 85%. Pulmonary function tests (PFTs) revealed an FEV1 of 0.39 liters (9% of predicted) and a FVC of 0.8 liters (16% of predicted).
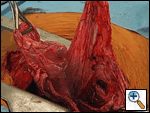
The patient returned to his baseline pulmonary status following continued medical and pulmonary therapy. It was apparent that the giant right-upper lobe bulla was causing compression of his pulmonary parenchyma and interfering with his pulmonary mechanics. Therefore, the patient electively underwent right thoractomy and stapling resection of the right-upper lobe bulla (Figure 3). There were several smaller bullae distributed in the remaining lung tissue, and these were not resected due to their diffuse nature. The resected specimen measured 9.5 cm x 5.5 cm x 4.0 cm, and represented benign lung tissue on pathologic examination (Figure 4). The patient had an uneventful post-operative recovery, and was discharged home on 2 liters nasal canula. Subsequently, he was able to be weaned-off home oxygen and his exercise tolerance improved.
 |
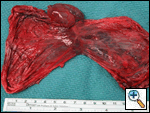 |
| Figure 3. Stapling resection of the right-upper lobe bulla | Figure 4. Resected specimen on pathologic examination |
Comments
Bullous lung disease is an uncommon cause of respiratory distress [1]. In patients with severe emphysema, discrete emphysematous bullae have been shown to functionally impair pulmonary mechanics and result in diminished exercise capacity and even acute respiratory distress [1-4]. Most patients with bullae have a significant cigarette smoking history, although cocaine smoking, pulmonary sarcoidosis, 1-antitrypsin deficiency, 1-antichymotrypsin deficiency, Marfan’s syndrome, Ehlers-Danlos syndrome and inhaled fiberglass exposure have been shown to be associated with emphysematous lung bullae [1-8].
Bullae which enlarge enough to compress adjacent lung tissue are best diagnosed by CT. A “double-wall sign” on chest CT, demonstrating air on both sides of the bulla wall, signifies an associated pneumothorax with the bulla [6]. In addition to chest CT, these patients should undergo ABGs and PFTs, The decision to operate is often a challenging one. Patients should undergo surgical resection when they have incapacitating dyspnea with large bullae that fill more than 30% of the hemithorax and result in the compression of healthy adjacent lung tissue [1]. In addition, operation is indicated for patients who have complications related to bullous disease such as infection or pneumothorax [1,4].
There are two surgical approaches for resecting giant lung bullae. Stapling resection of the entire bulla, either through a VATS or open approach, is the most common technique [1,4]. Pericardial strips can be used along the staple line to assist in control of air leaks since the surrounding lung tissue is often diseased. Another operative approach is the modified Monaldi technique, which involves opening the bulla, placing a purse-string suture at the neck of the bulla and closing the overlying bulluous sac with a running back-and-forth plicating stitch [8]. Both techniques have been shown to be effective. Smoking cessation and aggressive pulmonary rehabilitation are also important for successful treatment of patients with bullous lung disease.
References
- Greenberg JA, Singhal S, Kaiser LR. Giant bullous lung disease: evaluation, selection, techniques, and outcomes. Chest Surg Clin N Am 2003;13:631-49.
- Van der Klooster JM, Grootendorst AF. Severe bullous emphysema associated with cocaine smoking. Thorax 2001;56:982-3.
- Zar HJ, Cole RP. Bullous emphysema occurring in pulmonary sarcoidosis. Respiration 1995;62:290-3.
- Vigneswaran WT, Townsend ER, Fountain SW. Surgery for bullous disease of the lung. Eur J Cardiothorac Surg 1992;6:427-30.
- De Giacomo T, Rendina EA, Venuta F, et al. Bullectomy is comparable to lung volume reduction in patients with end-stage emphysema. Eur J Cardiothorac Surg 2002;22:357-62.
- Waitches GM, Stern EJ, Dubinsky TJ. Usefulness of the double-wall sign in detecting pneumothorax in patients with giant bullous emphysema. Am J Roentgenol 2000;174:1765-8.
- Snider GL. Reduction pneumoplasty for giant bullous emphysema. Implications for surgical treatment of nonbullous emphysema. Chest. 1996;109:540-8.
- Shah SS, Goldstraw P. Surgical treatment of bullous emphysema: experience with the Brompton technique. Ann Thorac Surg 1994;58:1452-6.



