ALERT!
This site is not optimized for Internet Explorer 8 (or older).
Please upgrade to a newer version of Internet Explorer or use an alternate browser such as Chrome or Firefox.
Thoracoscopic Sympathectomy
Patient Selection
Surgical interruption of intrathoracic autonomic neural pathways has several useful clinical applications, particularly thoracic sympathectomy for upper limb hyperhidrosis and splanchnicectomy for relief of pancreatic pain. The advent of video-thoracoscopy has lead to an explosion in the application of this minimally invasive technology for this purpose. Endoscopic thoracic sympathectomy (ETS) has been proved to be a safe technique, and the results in hyperhidrosis are rewarding, with a success rate of approximately 95% in most large series.1,2 Transthoracic division of the splanchnic nerves with vagotomy for the treatment of chronic pancreatitis was first reported in 1947 by Rienhoff et al.3 Thoracoscopic splanchnicectomy is a recently described approach that combines the benefits of a visually controlled division of the splanchnic nerves with a low complication rate and reduced patient discomfort.4,5 In our unit, ETS is mainly applied for patients with hyperhidrosis, however, its use in treatment of other sympathetic disorders, including splanchnic pain, reflex sympathetic dystrophy (RSD) and upper extremity ischemia, is also appropriate when non-surgical treatment fails.
Operative Steps
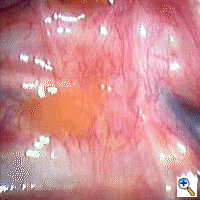
Surgical techniques: General anesthesia is used, including one lung ventilation with a double lumen endobronchial tube. CO2 insufflation is used to help induce lung collapse. A semi-Fowler's position is preferred with the patient's arms abducted and a roll behind the shoulders to improve access to the upper sympathetic chain (Figure 1). With gravity the lung naturally falls downwards and away from the upper posterior chest wall. Only one 7mm or 10mm port with an operative-thoracoscope is needed for manipulation. Alternatively, one telescope port and one operating port are placed if an operating thoracoscope is not available. The sympathetic chain is easily identified under the parietal pleura, running vertically over the necks of the ribs in the upper costo-vertebral region.
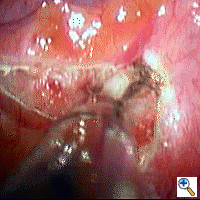
We perform bilateral synchronous sympathectomy starting on the right side. An L-shaped hook cautery alternating cutting/coagulation is used to divide the sympathetic chain as this is easier and quicker than attempting to remove a segment of the chain (Figures 2-4). Special care is taken to make sure that complete ablation of ganglia and severance of the sympathetic chain is achieved. We generally continue the dissection by cauterizing/dividing the pleura for 5 cm lateral to the chain. If an aberrant nerve bundle of Kuntz is identified, it too is severed. The transected ends of the sympathetic chain are separated as far as possible and cauterized to prevent regrowth of the nerve and recurrence of symptoms. For patients with hyperhidrosis, level T2 and T3 or T2-T5 are divided, depending on the severity of the lower extremity symptoms. Care should be taken not to divide the sympathetic chain above the level of the second rib for the treatment of palmar and plantar hyperhidrosis, because it increases the risk of Horner's syndrome and contributes little benefit. Thoracic outlet syndrome or reflex sympathetic dystrophy is usually approached at T1-T3. For chronic pancreatic pain, we usually divide the sympathetic chain at the level of T4 to T10. Before closing the skin, a small chest tube is left in the chest and the subcutaneous tissue is closed with 3-0 Vicryl. After expanding both the patient's lungs with positive pressure ventilation, the tube is removed from the chest quickly at positive pressure to avoid a residual pneumothorax, and then a final subcuticular suture is placed. Hence, no thoracic drain is needed postoperatively. The procedure is then repeated on the left side. A chest radiograph is immediately obtained after the operation in the operating room to ensure complete lung expansion. The operation is usually performed in an outpatient setting, and patients are discharged 6-8 hours after the operation.
Preference Card
Standard thoracoscopy set up:
- Operating scope: 0° 10mm/ 30° 10mm
- Trocar ports: 10mm
- Hook cautery: 3/5 m
Tips & Pitfalls
- Bovie cautery, rather than mechanical resection, is preferred to divide the sympathetic chain as this is easier and quicker.
- Take care to make sure that complete ablation of ganglia and severance of the sympathetic chain is achieved.
- Cauterize/divide the pleura for 5 cm laterally; in this way, if an aberrant nerve bundle of Kuntz is identified, it too is severed.
- Separate the transected ends of the sympathetic chain as far as possible to prevent regrowth of the nerve.
- Do not divide the sympathetic chain above the level of the second rib for the treatment of palmar and plantar hyperhidrosis; it increases the risk of Horner's syndrome and contributes little benefit.
- Use a scoring system with both subjective and objective components to measure the degree of sweating before and after surgery to evaluate the effectiveness of treatment. (Tables 1, 2)
Table 1: Severity of hyperhidrosis scoring system
| Grade 0 | Grade 1 | Grade 2 | Grade 3 | |
| Dampness | "None or Slight" | "Damp" | "Wet" | "Dripping" |
| Quality of Life | Normal | Annoyance | Debilitating | Social Phobic |
| Blot test | - | + | ++ | +++ |
Table 2: Severity of compensatory hyperhidrosis
| Grade 0 | Grade 1 | Grade 2 | Grade 3 | |
| Location | Any site | Plantar | Trunk | Facial |
| Dampness | "None or Slight" | "Damp" | "Wet" | "Dripping" |
| Quality of Life | Normal | Annoyance | Debilitating | Social Phobic |
Results
Sympathectomy has been described for the treatment of a wide variety of disorders. Dorsal sympathectomy or thoracic sympathectomy is usually performed for relief of hyperhidrosis, reflex sympathetic dystrophy (RSD), Raynaud's disease, and upper extremity ischemia, among other indications. Recent advances in endoscopic technology have led to the almost universal adoption of the endoscopic transthoracic route as the preferred technique for upper limb sympathectomy and have also rekindled interest in thoracic splanchnicectomy as a treatment for pancreatic pain. So far, however, most large series have been reported from Europe and the Far East; only few recent reports have originated from North America.6,7 We began using video-assisted thoracoscopy to do sympathectomy in 1992. Since then, we have performed ETS for treatment of a variety of sympathetic disorders including hyperhidrosis, splanchnic pain, reflex sympathetic dystrophy (RSD), and upper extremity ischemia.8
Palmar hyperhidrosis is the main indication for ETS in our center. We have performed bilateral ETS in 121 patients with palmar hyperhidrosis in an outpatient setting since 1992. There were 57 male and 64 female patients with a median age of 27 years (range from 9 to 73 years). The median hospital stay was 1/2 day (range 1/2-3). Postoperative complications occurred in 11 patients (9%; 11/121), which included chest hypersensitivity (3 cases), chest pain (2 cases), Horner's syndrome (2 cases), chylothorax (1 case), pneumothorax (1 case), arm pain (1 case), and chest numbness (1 case). All patients (100%) were satisfied with the immediate treatment effects on the preoperative symptoms of palmar hyperhidrosis. Forty-three (35.5%; 43/121) of patients with hyperhidrosis had mild compensatory sweating in areas of the trunk, back, inner thigh, or foot postoperatively. Ten patients (8.3%; 10/121) developed significant compensatory sweating, but only 2 of them (1.7%; 2/121) complained of intolerable symptoms.
Our other indications for ETS include facial blushing (6 patients), upper extremity ischemia (3 patients), splanchnic pain (2 patients) and reflex sympathetic dystrophy (2 patients). Preoperative symptoms resolved completely or improved significantly in 84.6% (11/13) of these patients. One patient with facial blushing and one patient with left reflex sympathetic dystrophy had recurrence of symptoms 2 months and one week after operation, respectively. Our initial results of the application of ETS in these patients seems encouraging; however, more cases and long-term follow up are needed to define the treatment effects for these indications other than hyperhidrosis.
In conclusion, ETS in an outpatient setting is a safe and effective procedure for treatment of hyperhidrosis. Its application for the treatment of other sympathetic disorders, although initial results seem encouraging based on our limited experience, needs to be further defined.
References
- Cohen Z, Levi I, Pinsk I et al. Thoracoscopic upper thoracic sympathectomy for primary palmar hyperhidrosis - the combined paediatric, adolescent and adult experience. Eur J Surg 1998;Suppl 580:5-8
- Olsson Rex L, Drott C, Claes G, et al. The Borås experience of endoscopic thoracic sympathicotomy for palmar, axillary, facial hyperhidrosis and facial blushing. Eur J Surg 1998;Suppl 580:23-26
- Rienhoff WF, Baxter BM. Pancreolithiasis and chronic pancreatitis: preliminary report of a case of apparently successful treatment by transthoracic sympathectomy and vagotomy. JAMA 1947;134:20-1
- Worsey J, Ferson PF, Keenan RJ, et al. Thoracoscopic pancreatic denervation for pain control in irresectable pancreatic cancer. Br J Surg 1993;80:1051-2
- Cuschieri A, Shimi SM, Crosthwaite G, et al. Bilateral endoscopic splanchnicectomy through a posterior thoracoscopic approach. J R Coll Surg Edinb 1994;39:44-7
- Krasna MJ, Flowers J, Mjorvik R. Thoracoscopic sympathectomy. Surg Laparosc & Endosc. 1993;5(3):391-394
- Krasna MJ, Demmy TL, McKenna RJ, et al. Thoracoscopic sympathectomy: the U.S. experience. Eur J Surg 1998;Suppl 580:19-21
- Krasna MJ, Jiao X, Sonett J, et al. Thoracoscopic sympathectomy. Surg Laparosc Endosc Percutan Tech 2000;10:314-318





Comments