ALERT!
This site is not optimized for Internet Explorer 8 (or older).
Please upgrade to a newer version of Internet Explorer or use an alternate browser such as Chrome or Firefox.
Endovascular Interventions on the Iliac Artery
Tuesday, January 18, 2011
Patient Selection
Indications for endovascular repair of the iliac artery are:
- Stenosis or (short-segment) occlusion of iliac artery (TASC type A and B, TASC C lesions are controversial) with ipsilateral lower extremity ischemia (lifestyle-limiting, progressive claudication, rest pain, gangrene).
- Patients with asymptomatic aneurysm greater than 4 cm in diameter.
- An iliac aneurysm which has also increased in size by 0.5 cm in last six months.
- Symptomatic iliac artery aneurysms mandate endovascular (or open) repair regardless of size.
- Patients with long occluded lesions/poor run-off/acute limb ischemia are poor endovascular candidates.
Operative Steps
- The patient is placed in the supine position. Both groins and the entire abdomen are prepped and draped. Artery Iliac interventions may be performed under general, regional or local anesthesia.
- Ipsilateral percutaneous common femoral artery access (retrograde approach) is obtained in majority of cases. In iliac lesions or aneurysms in distal external iliac artery, an antegrade approach is chosen. This involves coming from the contralateral common femoral artery using a crossover technique. In total occlusion, a combined ante-, and retrograde approach may be chosen. The brachial artery is accessed only if there is difficulty with femoral access or crossover technique
- The patient is heparinized for a target activated clotting time ≥ 200 sec. This level of anticoagulation is maintained throughout the procedure.
- After common femoral artery access using the Micropuncture set, a .035-inch x 180 cm starter guidewire is inserted to cross the iliac artery lesion/aneurysm. Alternatively, a .035 hydrophilic wire or a super-stiff Amplatz may be used to navigate the lesion.
- Initially a 6 F introducer sheath with distal is inserted over the primary access guidewire in the femoral artery. If aortic ballooning or IVUS is used a 9-12 F sheaths are necessary. A 5 F Bern or multipurpose catheter is introduced to facilitate guidewire exchange to a stiff wire (such as the Meier wire or Amplatz). This wire will straighten tortuosity of the access vessel and improve tracking capability of the introduced catheters and devices.
- The pigtail catheter (4-5 F) is used to perform an angiogram the aorta and iliac arteries.Contralateral caudal oblique angulations are very helpful in laying out the common and external iliac arteries. In addition, IVUS interrogation of the vessels may be performed at this time. The length and the diameter of the proximal and distal neck are measured using the angiogram, calibrated catheters or skin markers with or without the IVUS or CT measurements. Based on these measurements and the anatomy, the treatment plan is chosen, that may include balloon angioplasty versus stent grafting (self-expanding vs balloon-expandable vs covered stents).
- Simple iliac TASC type A lesions are treated with balloon angioplasty using .035-inch compatible angioplasty balloons with diameters of 5-10 mm and lengths between 20-40 mm. In distal aortic or bifurcation disease, a kissing balloon approach may be necessary (Figure 1). Indications for stenting include suboptimal results of angioplasty with residual gradients, extensive dissection, total occlusion, reoccurrence after angioplasty, ostial location, severe calcification as well as aneurysms. Most commonly balloon expandable stents are used that offer greater radial force, and greater precision for placement for ostial and calcified lesions. More flexible self-expanding stents offer better taper for longer lesions, and are used for antegrade approach, treatment of external iliac and common femoral lesions, and longer lesions. Finally stent grafts are commonly used for aneurysmal pathologies or vascular ruptures.
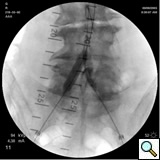 |
| Figure 1: Kissing balloon for proximal common iliac disease. |
- In aneurysmal pathologies, it is important to cover the entire length of the aneurysm. The stent grafts are subsequently ballooned as suggested by the IFU. An IVUS interrogation of the entire stent graft is a helpful adjunct. This will detect any circumferential stent mal-apposition to the proximal or distal landing zone that may lead to endoleak. A completion angiogram is performed to confirm lack of gross endoleak. However a single arteriogram may miss endoleak due to projection overlap. A bi-plane arteriogram is more reliable in excluding any significant procedural endoleak.
- After the completion angiogram, the introducer sheath is removed while carefully leaving the wire in the vessel. If the patient remains hemodynamically stable, an intact iliac/femoral artery may be assumed. In majority of cases and with percutaneous technique, manual compression or vascular closure devices are used. In case of open femoral artery exposure, the wire is removed, and the femoral artery is repaired in standard fashion.
- The distal pulses are checked. If they correspond to preoperative baseline, the heparin is reversed. At this time, the sterile endovascular wires/catheters may be disposed.
Preference Card
Sheaths
- 4-11 F with distal tip markers (Cordis Brite Tip 5.5 or 11 cm) sheath used for femoral access.
- 6-9 F sheath (Terumo 10cm Pinnacle Sheath) is may be used alternatively.
- 5 F sheath (Terumo 10cm Pinnacle Sheath) used for left brachial/radial artery if needed for body floss maneuver or contralateral limb gate cannulation.
- Large 12 or 14 F sheaths (Terumo Pinnacle or Cook Check Flo) should be available for post-deployment molding of the abdominal graft with large-diameter occlusion balloons.
Catheters
- 5 F Bern (Boston Scientific 5 F x 100 cm Imager II Selective- Berenstein tip) or angled tip catheter used for ipsilateral aortic access, or brachial/radial artery access.
- 5 F pigtail catheter (Cook, Inc. 5 F x 90 cm Pigtail-Royal Flush Plus) used in the contralateral femoral artery.
- Omniflush (Angiodynamics Angioptic, 4-5 F x 90 cm) may be used as flush diagnostic catheter or selective diagnostic catheter in retrograde approach in steep angulated aortic bifurcation.
- Cobra C1 or C2 (Cordis Tempo angiographic, 4-5 F x 80-100 cm) for broader angle bifurcation
- 8.2 F IVUS catheter (Volcano, 8.2 F x 90 cm Vision PV, 8-12 MHz).
Guidewires
- Bentson Starter guidewire (Boston Scientific 0.035-inch x 180 cm Starter).
- 180 cm hydrophilic guidewire J-curved (Terumo 0.035-inch x 180 cm Glidewire).
- 0.035-inch (or 0.025) x 180 cm Stiff type guidewire with soft tip (Boston Scientific 0.025-inch x 180 cm Platinum Plus ST Guidewire; Boston Scientific 0.035-inch x 180 cm Amplatz Super Stiff Guidewire, 6 cm tip length).
- 450 cm Hydrophilic guidewire (Terumo 0.035-inch x 450 cm Glidewire) for “flossing” and brachial access cases.
Balloons
- Angioplasty balloon (Boston Scientific Ultrathin Diamond Balloon, 2-6 cm length, 5-12 mm in diameter).
- Large diameter (~ 40 mm) compliant occlusion balloons (Medtronic 12 F Reliant Balloon, 46mm max diameter; Cook, Inc., 14 F CODA Balloon Catheter, 40mm max diameter) for distal aortic procedures or management of acute ruptures.
Stents
- A large variety of stents and stent grafts exists. This will be handled under “Nuts and bolts”!
Miscellaneous
- Dilator (Endovascular Dilator Set, Cook, Inc. 20-24 F).
- Snare (Medical Device Technologies 27-45 mm EN Snare).
- Luer-Lock (Boston Scientific FloSwitch HP).
- Needle for initial arterial access Micro-Puncture Introducer Set (Cook, Inc. 4 F, MPIS-401).
- Torque device ( Terumo Torque Device).
- Proglide Suture-Mediated Closure Device (Abbott Vascular, 5-8 F access sites).
Tips & Pitfalls
- Iliac artery interventions are an essential skill for the endovascular specialist to master for multiple reasons. Beside improving blood supply to the lower extremities, preservation of vascular access for other endovascular procedures such as TEVAR, coronary angiogram, percutaneous valvular therapies, insertion of IABP, and to treat vascular access complications.
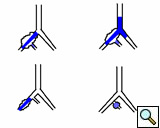 |
| Figure 2: Various locations of iliac artery aneurysms and stent placements |
- Isolated iliac artery aneurysms are rare (Figure 2). Isolated internal iliac artery aneurysms are embolized. Pre-procedural embolization of internal iliac artery may also be necessary to prevents retrograde filling of the aneurysmal sac and late rupture. In case of aneurysm of distal part of external iliac artery contralateral access is gained and followed by a cross-over technique. This is done because the femoral access site will either be too close or may itself be part of the aneurysm. Same access applies for sub-intimal dissections and iliac occlusive disease in distal part of the external iliac artery. Majority of iliac aneurysms are accompanied with infra-renal aortic aneurysms that need to be treated concomitantly. Similarly, common iliac artery and proximal external iliac without proximal neck necessitates stent graft placement in the aortic bifurcation (Figure 3).
- Navigating a very narrow or long stenotic lesion as well as cannulation of the contralateral limb gate is the portion of the operation that requires the most “wire skills”. This portion may become lengthy and discouraging if the surgeon fails to cannulate the gate using a particular approach. The authors recommend setting a specific time period for retrograde cannulation of the contralateral gate, and to proceed to the next step (antegrade or crossover cannulation) once this time has elapsed. The brachial/artery approach is the next step in the algorithm.
- IVUS is an important adjunct of iliac interventions. It is used in cases with “diagnostic dilemma” in which the noninvasive results or the symptoms do not match the angiographic findings. It helps with lesion severity, accurate vessel sizing, virtual histology, aneurysmal pathology as well as complex bifurcation disease.
- If there is doubt about hemodynamic significance of an angiographic finding, it should be assessed by intra-arterial pressure measurements across the lesion at rest and with induced hyperemia. Peak systolic difference of 10 mm Hg or less pre-vasodilatation, and 15 mm Hg post-vasodilatation are thresholds for a significant stenosis.
- While simple TASC type A may be optimal endovascular cases for the novice endovascular surgeon. The skills necessary to perform complex iliac interventions can not be attained through short “courses.” A dedicated formal training (six months minimum!) is necessary in order to obtain the “wire skills” and to independently perform these endovascular procedures. The trained endovascular surgeon should be able to deal with intraoperative complications of iliac intervention including extensive dissection and rupture. Peripheral artery angioplasty/stenting should be part of the armamentarium of the endovascular surgeon. The current privileging criteria in most tertiary hospitals require a minimum of 100 diagnostic, 50 interventional procedures to become certified/privileged in peripheral interventions.
- Most cardiothoracic surgeons will not meet the above training criteria (see also the credentialing section in the Endoluminal Technology Portal). In these cases, the necessary “wire skills” may be acquired by hiring a cardiothoracic surgeon who has had dedicated training in endovascular surgery. Alternatively, collaboration with other physicians with interventional skills (vascular surgeons, interventional radiologist/cardiologist) will be crucial.
- Train a dedicated nursing team for your endovascular cases. An Endosuite will substantially improve your imaging capabilities and broaden your endovascular options.
- All patients are placed on aspirin for 30-60 days unless there is a contraindication. Clopidogrel is not required for iliac interventions, but may be used as alternative to aspirin.
References
- Schneider PA. Endovascular Skills, 3rd Ed. New York: Informa 2009.
- Peripheral Endovascular Interventions. White RA, et al.; New York: Springer; 1999.
- Norgren L, Hiatt W, DormandyJ, et al. Inter-Society Consensus for the Management of Peripheral Arterial Disease (TASC II). J Vasc Surg 2007;45:S5-67.
- Mastery of Vascular and Endovascular Surgery. Zelenock GB, et al.; Philadelphia: Lippincott Williams and Wilkins; 2006.
- Manual of Peripheral Vascular Intervention. Casserly IP, et al.; Philadelphia: Lippincott Williams and Wilkins; 2005.
- Endovascular Therapy: Principles of peripheral intervention. Lumsden AB, et al Malden: Blackwell Futura; 2006.
- Vascular medicine and endovascular interventions. Rooke TW et al [Editors]; Malden: Blackwell Futura 2007.
- Vascular and endovascular surgery. Moore WS [Editor]; Philadelphia: Saunders; 2006.