ALERT!
This site is not optimized for Internet Explorer 8 (or older).
Please upgrade to a newer version of Internet Explorer or use an alternate browser such as Chrome or Firefox.
Featured Profile and Interview With Karen Redmond, MD
Professor Karen Redmond is a specialist thoracic lung transplant surgeon with an interest in minimally invasive surgical approaches, treating patients with end-stage lung disease, lung cancer, and conditions such as pectus and complex airway conditions. She began her medical education at University College Dublin, where she received an honors degree with the Gold Medal in Surgery. She then proceeded to win the prestigious Society Medal from the Society for Cardiothoracic Surgery in Great Britain and Ireland and completed special training in cardiothoracic surgery in 2007. After being awarded a minimally invasive lung cancer surgery scholarship and training in her subspecialty field at Toronto General Hospital, Canada, she went on to become the first female lung transplant surgeon in the British Isles.
Dr. Redmond has been integral in a variety of pioneering techniques. She has international expertise in ex-vivo lung perfusion, being the surgical principal investigator for the UK Develop Trial. As one of the first trained robotic surgeons with a recently published comparative meta-analyses on robotic lobectomy and thymectomy, she is also one of the first thoracic surgeons worldwide to start an iVATS program, which involves resecting pulmonary nodules supporting diagnosis or curative resection of pulmonary metastases.
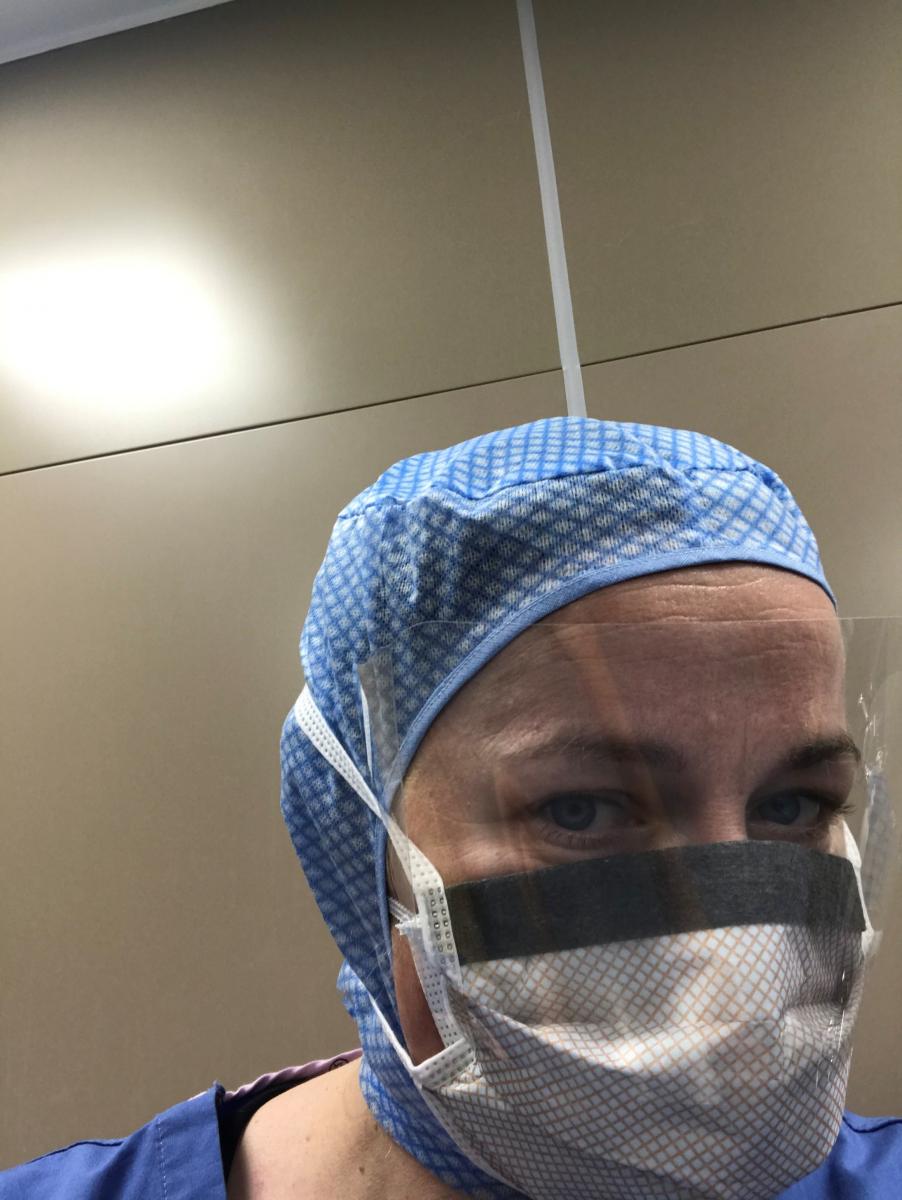
Wearing a washable surgical hood hand sewn by a theater nurse to support resterilization of PPE during the COVID-19 crisis.
After consulting at the Royal Brompton and Harefield Trust in the UK, Professor Redmond returned to Dublin, Ireland, in 2011 to expand the thoracic surgery and national lung transplant unit at the Mater Misericordiae University Hospital. She currently lives in Dublin with her family, including three young children.
Dr. Redmond is a member of CTSNet and a number of international societies and advisory groups, including the Society for Cardiothoracic Surgery in Great Britain and Ireland. She runs a postgraduate academic program supporting MDs and PhDs seeking to complete their interest topics in pulmonary rehabilitation, health economics, and EVLP.
Catherine Joyce for CTSNet:
CTSNet: You trained in thoracic surgery and lung transplantation in Canada, consulted in the UK, and ultimately returned to Ireland. What was the most interesting or valuable aspect of practicing in a different country?
KR: I was lucky enough to be mentored by internationally renowned surgeons, leaders in medical innovation, who delivered exceptional care to patients with complex thoracic conditions. Although the healthcare systems in these countries are different, there was commonality in how well staff communicated and respected each other, always remaining professional with an emphasis on research, audit, and quality initiatives. I would like to think that I have built my service around such experiences that strive to provide the highest standard of care.
CTSNet: What is the biggest challenge facing minimally invasive thoracic surgery right now?
KR: In 2018, I published a systematic review and meta-analysis qualifying robotic lobectomy as a reasonable alternative to VATS with superior short-term survival. However, evidence-based commissioning of robotic services is required to expand international programs. One of my postgraduates, with the support of a medical statistician and health economist, has just completed a manuscript for submission documenting costs.
CTSNet: What changes have you seen for women in cardiothoracic surgery since becoming the first female lung transplant surgeon in both the UK and Ireland?
KR: There are more women taking up consultant posts and achieving their career aspirations, whilst spending time on themselves, with their partner, and children. I would like to see more women promoted to leadership roles in an effortless way.
CTSNet: You have used pioneering techniques and have extensive general thoracic surgery experience. What is your favorite procedure? Why is it your favorite?
KR: Lung transplantation! Although cases can be grueling at times, having experience, judgment and operative skills delivers a good surgical result. It is so rewarding to deliver a second chance of life for patients with debilitating dyspnea.
CTSNet: If you had a magic wand to create the next innovation in CT surgery, what would it be?
KR: I am currently looking into assessing techniques to denervate large airways using my ex-vivo lung perfusion model. Such treatments may facilitate airway stenting not always tolerated by patients with such conditions as tracheobronchomalacia. I have lots of ideas!
CTSNet: Thank you, Dr Redmond!