ALERT!
This site is not optimized for Internet Explorer 8 (or older).
Please upgrade to a newer version of Internet Explorer or use an alternate browser such as Chrome or Firefox.
Featured Profile and Interview With Peyman Sardari Nia, MD, PhD

Dr Peyman Sardari Nia is a Senior Consultant Cardiothoracic Surgeon in the department of cardiothoracic surgery at Maastricht University Medical Center, the Netherlands, where he specializes in minimally invasive cardiothoracic surgery. Dr Sardari Nia earned his MD and his PhD from University Antwerp, Belgium, and underwent residency training in general surgery in the same city. Dr Sardari Nia was awarded the Pfizer educational prize in 2009: this prize is bestowed by the University of Antwerp on one young specialist for excellence in clinical, scientific, and surgical qualities during his or her whole residency across all the surgical specialties. Following his residency in general surgery, Dr Sardari Nia underwent a fellowship training in cardiothoracic surgery at St Antonius Hospital in Nieuwegein, the Netherlands.
Dr Sardari Nia’s PhD research focused on prognostic factors of lung metastases and non-small cell lung cancer, particularly how tumor growth patterns can inform post-surgical outcomes. He has received multiple awards for his research, notably the American Association of Cancer Research scholar-in-training award and European Association for Cardio-Thoracic Surgery (EACTS) Young Investigator award. His current research is focused on preoperative planning by use of 3D imaging reconstruction, 3D printing, simulation, and intraoperative navigation. He received the EACTS Techno-College Innovation Award for his invention of the high-fidelity endoscopic mitral valve surgery simulator.
Dr Sardari Nia is an all-around cardiothoracic surgeon with special interest in surgery for lung cancer and minimally invasive adult cardiac surgery, especially endoscopic mitral valve repair and VATS lobectomy. In addition to introducing and innovating minimally invasive approaches at his home institution, he is the founder and director of the EACTS courses in minimally invasive techniques for adult cardiac surgery and endoscopic mitral valve repair, using the high-fidelity simulator that he developed. He has been an EACTS councilor and a member of various EACTS committees since 2008. He is an associate editor of European Journal of Cardio-Thoracic Surgery (EJCTS) and a member of EACTS, The Society of Thoracic Surgeons, and the International Society for the Study of Lung Cancer.
Claire Vernon for CTSNet: How has the research you’ve done shaped how you approach your clinical practice?
Dr Peyman Sardari Nia: I am of opinion that there is a lot of pseudo-science and craftsmanship within cardiothoracic surgery, resulting in the quality of our interventions being very dependent on an individual surgeon’s performance. We are, in a sense, operating in a twilight between art and science. Art is about uniqueness, and science is about reproducibility. We surgeons all want to excel and perform surgeries that are both unique and of superior quality, but what is important is to have reproducibility in quality in the hands of as many surgeons possible for as many patients as possible. My current research concerns the preoperative planning for both cardiac and thoracic operations. The concept of preoperative planning involves using new technologies such as 3D imaging reconstruction, 3D printing, simulation, and intraoperative navigation to enhance the safety, efficacy, and reproducibility of cardiothoracic interventions. These projects have really changed my clinical practice, as I am using these tools on a daily basis to plan my operations, and also to show in ongoing studies the value of these tools for other surgeons.
CTSNet: Can you tell us more about the value of viewing the operation in three dimensions prior to entering the operating theater?
PSN: During my residency, my supervisor would ask me before entering the OR whether I had done the operation already in my head. In a sense, this was a kind of preoperative planning. Nowadays we have technology that enables us to create a hologram of the operative field and go through it layer by layer. Our operations are composed of many technical steps, and their outcomes are logically dependent on an individual surgeon’s experience and individual patient’s anatomy. Even an experienced surgeon doing routine operations on a daily basis would experience that the same operation is more difficult in some patients than others, according to each individual patient’s anatomy. Three-dimensional reconstruction and 3D printing enables us to have the knowledge of exact surgical anatomy preoperatively, and to draw a surgical plan to address the anatomical variabilities to enhance the safety, efficacy, and reproducibility of our surgical procedures. Additionally, the surgical anatomy is crucial for planning minimally invasive cardiothoracic surgical procedures, whereby we perform the same operations through smaller incisions (minimal access) or with new concepts (transcatheter, beating-heart, etc). We are also moving away from pathology-based interventions towards individualized interventions, with the central question being which patients will be suitable for which surgical technique, rather than which technique is superior? To answer this question for individual patients, we need the exact knowledge of individual surgical anatomy.
CTSNet: Can you tell us more about your endoscopic mitral valve simulator and the value in being able to “dry lab” a minimally invasive mitral valve repair?
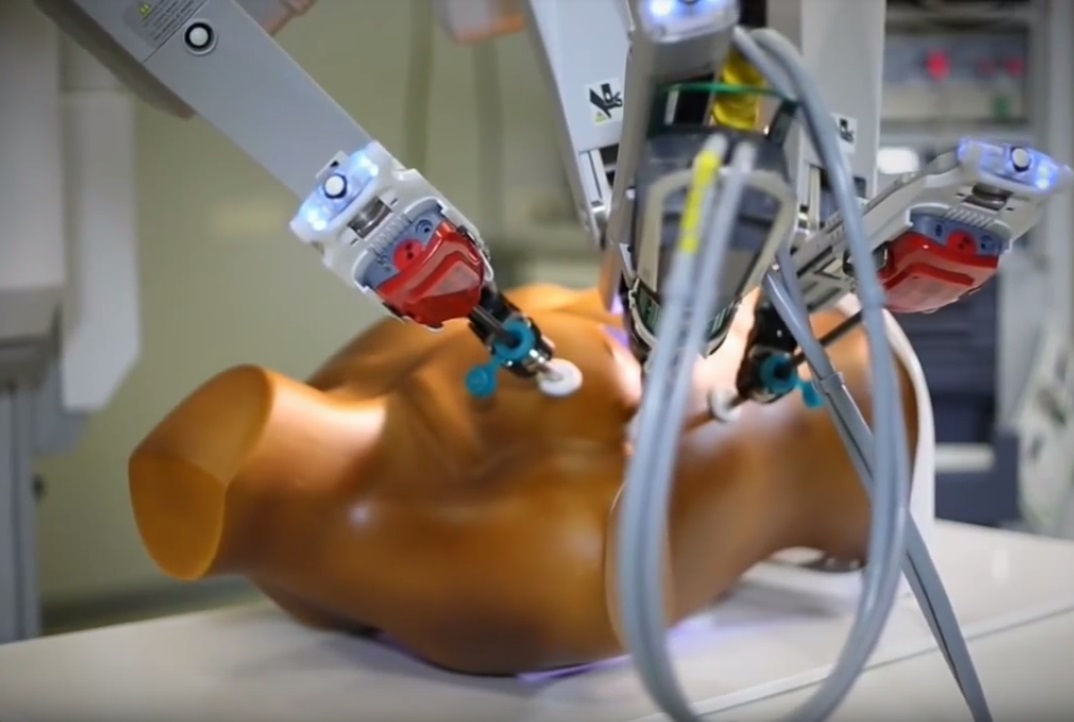
A robot works on Dr Sardari Nia's endoscopic mitral valve simulator.
PSN: Endoscopic mitral valve repair is one of the most difficult procedures to learn. The learning curve is steep. This steep learning curve has “partially” to do with the fact that the operation is done with long-shafted instruments, with surgeon looking at the monitor rather than into the wound. Acquiring endoscopic skills with long-shafted instruments is a process that no one can escape from. Acquiring these skills in patients is not logical or efficient. The simulator provides a platform to train the endoscopic skills repeatedly and objectively. Additionally, the simulator provides objective assessment and feedback, which is essential in any simulator-based training. Also, the disposable mitral valve is made of special silicone developed by us that provides a true suturing experience. We have developed a disposable 3D-printed pathological silicone replica that can be mounted into the simulator so that one can also be trained in any repair technique on any pathology of the mitral valve. The simulator can be used for training purposes, for preoperative planning of complex cases, and for facilitating the start of a new program.
The simulator can also be used for robotic-assisted mitral valve repair or minimally invasive mitral valve repair with direct vision. The simulator is used in EACTS’s endoscopic mitral valve repair courses that I direct four times a year at the Maastricht University Medical Center. The course is designed like an air-pilot-training concept course, starting with technical and theoretical pre-assessment and two subsequent days of intensive training on simulators, mixed with interactive presentations and videos regarding all aspects of the endoscopic mitral repair program. The course ends with technical and theoretical post-assessment. We have already trained over 100 surgeons, and our preliminary analyses show very promising results for skill development using the simulator.
CTSNet: How does the concept of personalized medicine fit into treatment for valve disease?
PSN: We introduced the concept of personalized medicine for mitral valve disease in an article published at the beginning of 2017 (Sardari Nia, 2017). This concept has three pillars:
- Concentrating on the whole process of treatment from the pre-treatment phase to the post-treatment phase. So, not focusing exclusively on the operation.
- Working with dedicated teams throughout the pre-treatment phase to the post-treatment phase. Why dedicated teams? Because we know from a plethora of publications that there is a direct association between volume and outcomes across all surgical procedures, and especially for mitral valve disease.
- Preoperative/pre-treatment planning: using the new technologies of 3D imaging reconstruction, 3D printing, and simulation in a dedicated mitral valve heart team to evaluate the treatment option to which patients are most suited.
Once again this concept is to enhance the quality of care by enhancing the patient safety, efficacy, and reproducibility of our treatments. In an ongoing prospective study, we will provide evidence of the merits of this new concept.
CTSNet: The “heart-team” concept, the close collaboration of cardiac surgeons and cardiologists in the performance of procedures such as TAVR, continues to gain importance with the growing significance of minimally invasive procedures. What is the future of the heart-team approach in treating patients with cardiac diseases?
PSN: We have a very unique position in the Netherlands because we have institutionalized the heart team. No patient undergoes any cardiac operation without the consent of the heart team in the Netherlands. In Maastricht, we have moved this one step further. No patient in our hospital or in the regional referring hospitals undergoes any kind of elective cardiac intervention without the consent of the heart team. Even one-vessel disease is discussed by the heart team. Additionally, we have created super-specialized heart teams for mitral valve, TAVI, aortic surgery, and AFib treatment, bringing experts on each field together to work out a treatment strategy. I believe that an individual surgeon or cardiologist should not make the decision of any intervention on their own, as they may be biased to provide only the treatment in which they have expertise, rather than what is the best treatment option. The heart team provides a platform of different opinions and perspectives that will only benefit the decision-making process. I hope that the heart-team concept becomes one of the quality indicators of any hospital, anywhere in the world, providing treatment for cardiac diseases.
CTSNet: If you had a magic wand to create the next innovation in CT surgery, what would it be?
PSN: Scientific and technical advances are surpassed by time, but what are enduring are the conceptual changes. Therefore, if I had a magic wand, I would accelerate the transition of craftsmanship to smart surgery in our field by use of new concepts such as personalized medicine, preoperative planning, and the heart-team approach. The way we train our residents and ourselves is also very important. The training in procedures should be completely changed to be similar to how pilots are trained to fly aircrafts: by use of intensive, procedure-by-procedure, simulation-based skill development, with subsequent hands-on experience in patients with clear, measured objectives.
CTSNet: What is your favorite thing about CTSNet?
PSN: CTSNet provides an updated view of the current status in cardiothoracic surgery across the world, and this is my favorite thing about CTSNet. It gives us the opportunity to peek into the practice of our colleagues around the world and learn from each other.
Reference
Sardari Nia P, Heuts S, Daemen J, et al. Preoperative planning with three-dimensional reconstruction of patient's anatomy, rapid prototyping and simulation for endoscopic mitral valve repair. Interact Cardiovasc Thorac Surg. 2017;24(2):163-168.





Comments