ALERT!
This site is not optimized for Internet Explorer 8 (or older).
Please upgrade to a newer version of Internet Explorer or use an alternate browser such as Chrome or Firefox.
3D Printing in Thoracic, Congenital, and Cardiac Surgery
Background and Aims
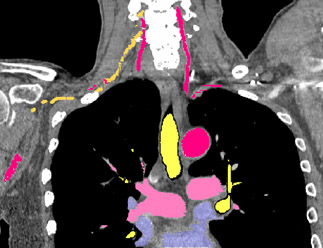
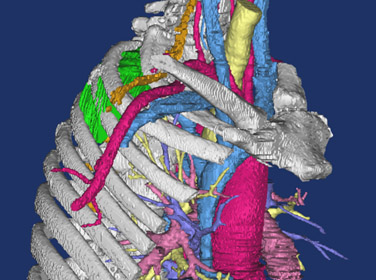
In complex cases, standard two-dimensional (2D) computed tomography (CT) images have limitations in their ability to demonstrate anatomical relationships in preparation for surgery. Three-dimensional (3D) printed anatomic models, using imaging data from high resolution CT scans, provide higher-level understanding of potential anatomic challenges. This is particularly true in patients with complicated past surgical history or pathology. Due to the unique characteristics of the esophagus, specialized techniques are necessary to enhance the quality of the 3D printed model of the esophagus.
Three-dimensional printing of anatomic models for complex surgical cases improves patient and resident education, operative team planning, and guides surgical resection. Incorporating additional patient factors, such as tumor response to therapy, into the model enhances its utility. Creating models with these five dimensions (5D) is also described.
Methods
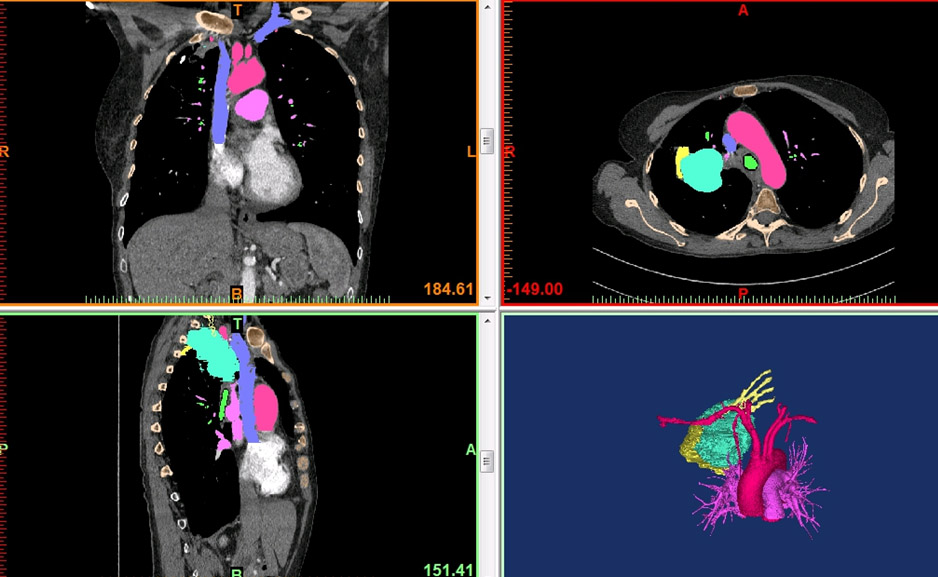
The Mayo Clinic, Rochester, Minnesota, has utilized 3D printing since 2006, with over 130 models printed throughout all surgical specialties. For patients with complex esophageal pathology, a unique application of an oral effervescent agent is combined with a positive enteric contrast agent to distend the esophageal lumen during CT scanning in order to facilitate esophageal segmentation during post-processing. This optimizes visualization of abnormal esophageal anatomy and the relationship to adjacent mediastinal structures. 3D anatomic models are printed using imaging data from each individual patient’s CT scans. The data is segmented and processed using proprietary software, and then converted into a stereolithography (STL) file. The STL file is sent to the 3D printer (Stratasys Connex 350 polyjet), and a model is created using liquid polymers. The reconstructions are used for multi-disciplinary pre-operative discussions, surgical planning, and as part of the patient education and consent process.
The process of 5D printing was developed to incorporate change in tumor size after neoadjuvant therapy in anatomic models used for surgical planning. Pre-treatment CT and PET scans are reformatted and fused. Crucial anatomy from these studies, along with post-treatment CT and MR, are coregistered. The fused anatomy is converted into stereolithography(STL) files for 3D printing.
Results
This video presents the utility of 3D printing to individualize management of complex esophageal pathology in two recent patients. The author performed a combined endoscopic and surgical procedure in a male patient with metastatic teratoma leading to a left pneumonectomy, complicated by an esophago-aortic fistula requiring aortic bypass and esophageal diversion without resection. 3D printing enabled visualization of his native esophagus, and allowed EMR of his esophagus via a transgastric stent with concomitant hiatal dissection, and transection of the GEJ. He recovered well, and esophageal reconstruction is planned. In the second patient, 3D printing allowed enhanced visualization of multiple esophageal diverticula in order to plan for the most appropriate surgical approach. The proximal extent of the diverticula was determined and the relationship to surrounding anatomy better elucidated.
A patient presenting with a complex thoracic tumor was selected for trial 5D printing. 3D and 5D models were prepared to allow surgical teams to directly evaluate and compare the added benefits of information provided by printing in 5D.
Conclusion
3D printed anatomic models are valuable tools when endoscopic or surgical intervention is planned in patients with complex esophageal pathology or anatomy. The author recommends ingestion of an oral effervescent agent in order to optimize the quality of esophageal imaging for these models, allowing for full appreciation of anatomical relationships. The printing of 3D anatomic models allows all members of the multi-disciplinary team to plan for the appropriate surgical approach, prepare for the intervention, and anticipate potential difficulties. The models also give each patient invaluable insight into their condition, and allow them to be fully involved in complex discussions regarding their care.
Printing 5D models in patients with complex thoracic pathology facilitates surgical planning, selecting margins of resection, anticipation of potential difficulties, and education for residents and patients.






Comments