ALERT!
This site is not optimized for Internet Explorer 8 (or older).
Please upgrade to a newer version of Internet Explorer or use an alternate browser such as Chrome or Firefox.
The Folding Leaflet Technique for Neochordal Repair in Barlow´s Syndrome: Step-by-Step
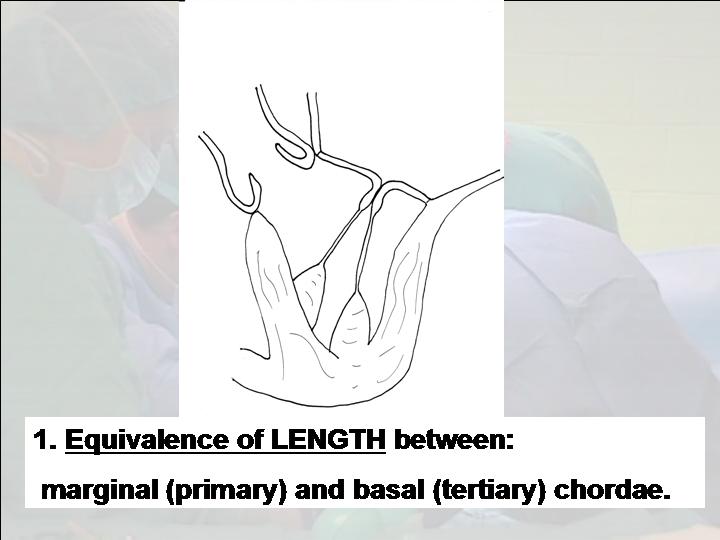
Figure 1. Equivalence of length between marginal
(primary) and basal (tertiary) chordae.
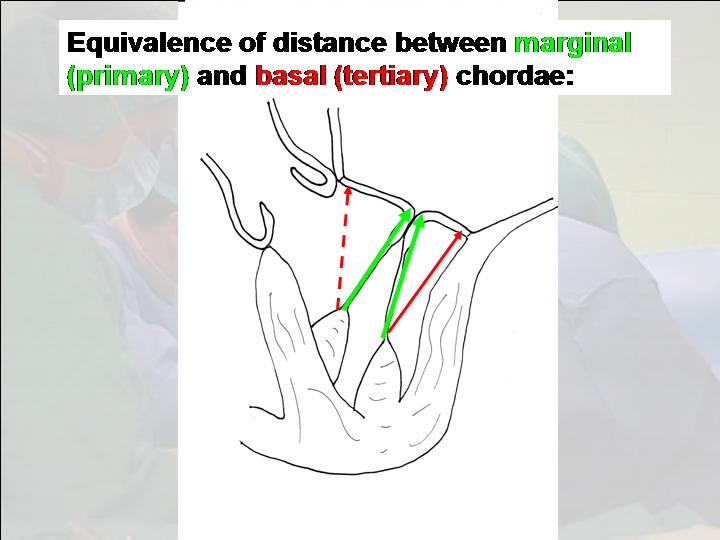
Figure 2. Equivalence of length between marginal
(primary) and basal (tertiary) chordae during left
ventricular systole.
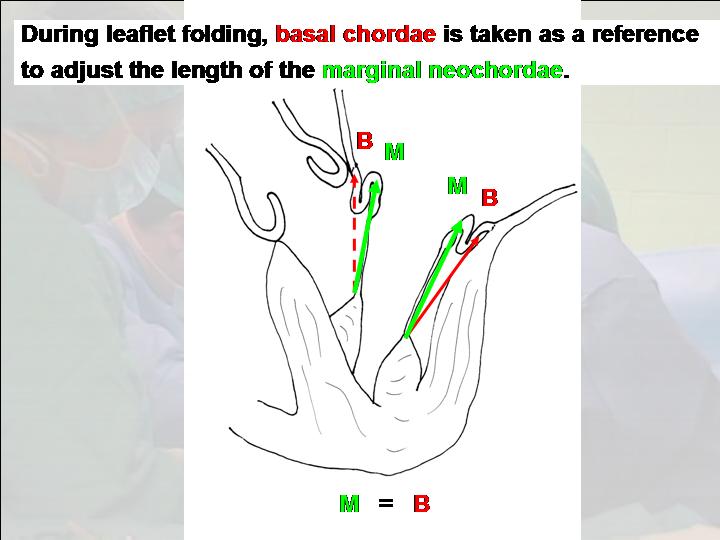
Figure 3. Equivalence of length between marginal
(primary) and basal (tertiary) chordae during
leaflet folding.
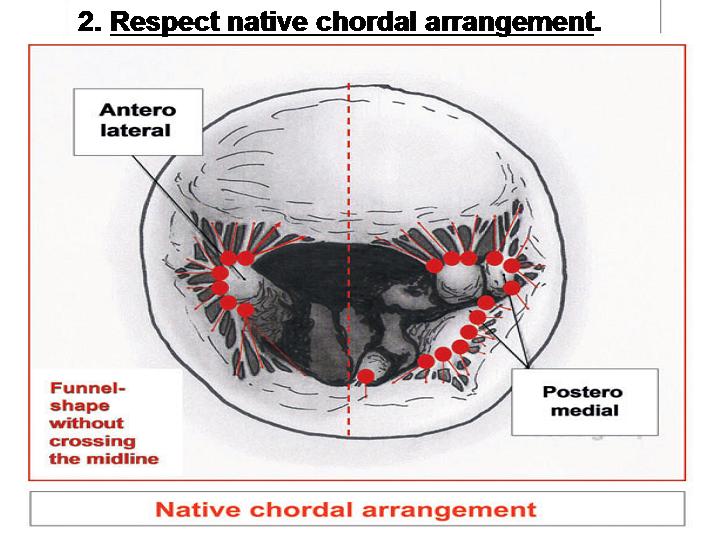
Figure 4. Respect native chordal arrangement.
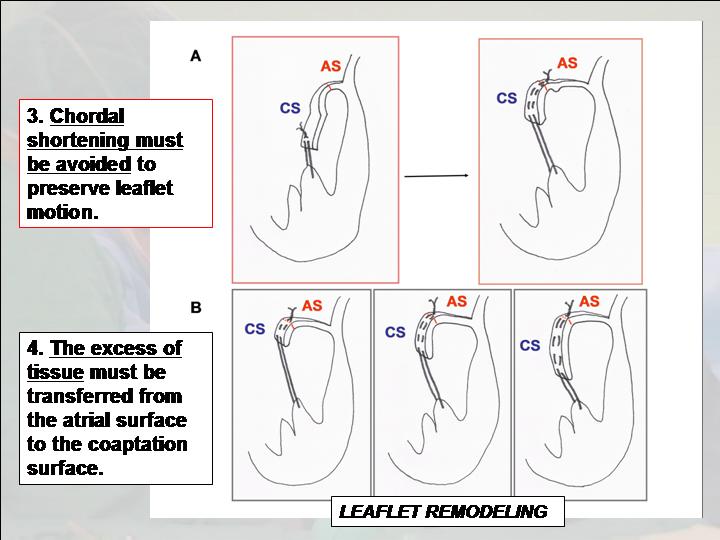
Figure 5. Avoid neochordal shortening to preserve leaflet
motion. The excess of tissue must be transferred from
the atrial surface to the coaptation surface in order to avoid
SAM.
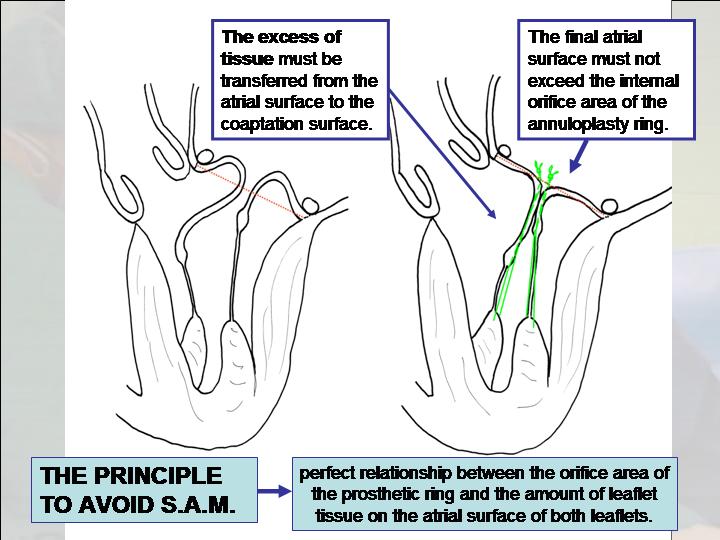
Figure 6. The method to avoid SAM.
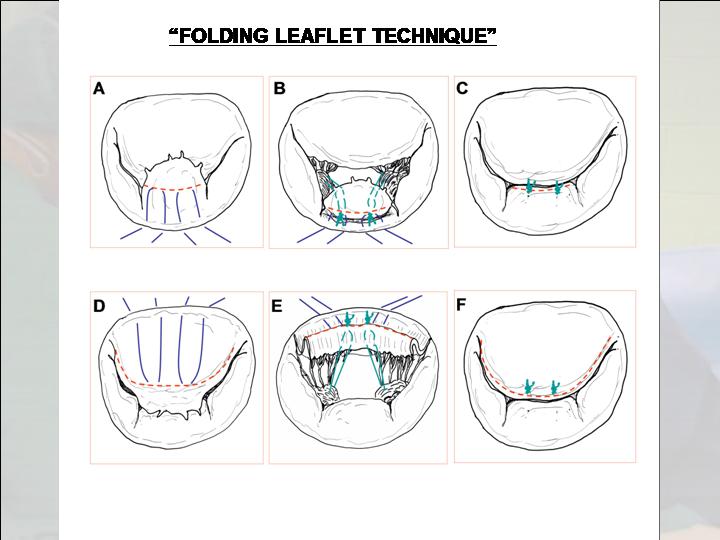
Figure 7. The folding of both leaflets.
The Challenges of Extensive Neochordal Repair in Case of Large Areas of Leaflet Prolapse
Despite the fact that neochordal repair is becoming increasingly popular, a number of challenges remain such as: the determination of the correct chordal length to ensure optimal leaflet coaptation, and the anchoring method of the artificial chordae to both papillary muscles and leaflets. In patients with large areas of prolapse, implantation of large numbers of neochordae is frequently necessary. In this setting, the drawbacks and limitations of some neochordal repair techniques are greatly enhanced. Several important operative steps must be considered by most of neochordal repair techniques: attachment of the chordae to the corresponding papillary muscle, attachment to the prolapsing leaflet, height modulation of the neochordae with tying knots, and implantation (or not) of an annuloplasty ring. Unsuccessful repair might be the consequence of any technical failure during the performance of these operative steps. This must stimulate the development of technical solutions for the extensive use of neochordae in order to apply them to different anatomical situations and to ensure their correct length, even in the absence of a reference point on a nearby segment of normal valve.
The authors’ aim was to overcome most of these potential limitations through a simple and effective technique: the “Folding Leaflet.” This procedure simplifies the use of multiple neochordae (ensuring the correct length), enhances leaflet coaptation, and promotes the maintenance of the functional anatomy of the valve. The authors describe the most important conceptual principles and technical issues related to this new approach in this step-by-step surgical video.
Surgical Technique: The Folding Leaflet
The operative technique for mitral valve (MV) repair utilizing the Folding Leaflet technique is based on the respect rather than resect approach postulated by Perier et al. This technique focuses not only on the creation of a large surface of coaptation, but also on preservation of normal leaflet motion. According to this last objective, transformation of the posterior leaflet into a vertical immobile buttress, as described by Perier, is avoided.
Basic Principles
- Equivalence of length between marginal (primary) and basal (tertiary) chordae (Figures 1, 2, 3).
- Respect native chordal arrangement (Figure 4).
- Avoid neochordal shortening to preserve leaflet motion (Figure 5).
- The excess of tissue must be transferred from the atrial surface to the coaptation surface in order to avoid SAM. (Figure 5, 6).
Step-by-Step Operative Points
- The neochordae are first fixed to the corresponding papillary muscle with a simple stitch without pledgets or tying, in order to simplify the technique and to preserve the papillary muscle integrity as much as possible. 4-0 Gore-Tex sutures are preferred in most patients. Neochordal repair should reproduce the native chordal arrangement (Figure 4). The correct papillary muscle group and unit must be selected to avoid crossing the midline when the neochord is implanted at the level of the corresponding leaflet.
- The two arms of each neochordae are passed through the free margin of the prolapsing leaflet in two or three full-thickness bites. Weaving this suture from the free edge and surpassing the coaptation line produces a free-edge remodelling, resulting in a “hockey-stick” effect on the leaflet, enlarging the surface of coaptation (Figure 5).
- The principle of basal-marginal chordae equivalence is also considered. The height of a marginal chord is equal to that of the corresponding basal chord (Figure 1, 2, 3). A pliable leaflet can be folded, and its free margin can be temporarily approximated edge-to-edge to the adjacent annulus that is used as the reference point while the neochord is tied. In this position, the length of the neochord will correspond to the height of the basal chord. After unfolding of the leaflet, the neochord will recover its marginal position and the adjusted basal height will turn into the equivalent marginal height. Its final length will exactly match the plane of the annulus at the coaptation point (Figure 7).
- In case of excess of tissue, the coaptation line must be moved closer to the annulus. The height of both leaflets can be reduced, without any resection, by moving the excess of tissue from the atrial to the coaptation zone during neochordae implantation. This is achieved weaving the Gore-Tex suture from the free edge, and surpassing the new coaptation line that has been moved closer to the annulus (Figure 5). In order to avoid systolic anterior motion of the MV (or SAM), the final atrial surface of the MV must not exceed the internal orifice area of the annuloplasty ring and the height of the posterior leaflet must be ≤ 2cm (Figure 6). Importantly, shortening of neochordae is avoided in order to preserve leaflet mobility.
- A complete annuloplasty ring must be implanted in all patients. The size of the annuloplasty ring must be selected according to the intertrigonal distance and the height of the anterior leaflet. “Water test,” before and after implantation of the annuloplasty ring and intraoperative transesophageal echocardiography must be routinely used.
Clinical Impact: Development of New Technical Solutions for Facilitating Extensive Neochordal Repair
Neochordal repair has been validated clinically over the past 2 decades and has become an increasing component of the surgical armamentarium for MV repair. This procedure appears to be safe, effective, and can be applied to a variety of anatomic situations providing stable functional results. But, irrespective of the particular details of the selected technique for MV repair, there are a number of important issues that must be applied to any use of artificial chordae.
- The minimum number of bites should be used when attaching the chord to the papillary muscle as this prevents tissue damage. Chordae should be attached to the fibrous head of the papillary muscle, using the minimum number of pledgets, to prevent papillary muscle ischemia. Our technique aims at avoiding damage to the head of the papillary muscle by attaching the chord with a single pass of the PTFE suture without tying or using U-stitches or pledgets. This procedure is simple and safe and may be especially important when a large number of neochordae are implanted.
- It is important to avoid passing the chordae across the midline, thereby respecting the anatomical chordae-leaflet pattern. Ideally the anatomical relation between the papillary muscles and the MV leaflets must be maintained. This means preserving the relationship between chordae from the anterior papillary muscle to the lateral half of the anterior and posterior leaflets, and between the posterior papillary muscle and the medial half of the anterior and posterior leaflets. In order to achieve a successful repair, the chordae should not cross these anatomical boundaries. The present technique also reproduces the native chordal arrangement. The correct papillary muscle group and unit are carefully selected to avoid crossing the midline when the neochordae are implanted at the level of the corresponding leaflet.
- Chordal attachment to the leaflet is also an important operative step. A number of different methods have been described for fixing the neochordae to the leaflet. This procedure usually involves securing the chord to the free edge of the prolapsing leaflet, avoiding tearing of tissue, while at the same time, making a neochord of a specific length. It must be considered that PTFE sutures are very slippery and the final length may vary at the time of knot tying. In the Folding Leaflet technique, the neochordal attachment to the leaflet aims to fix the PTFE suture and remodel the leaflet, creating a large surface of coaptation. In the case of excess of tissue, the chord is repeatedly woven along the surface of coaptation, reducing the atrial surface of the leaflet to the correct level. Basically, the excess of leaflet tissue is moved from the atrial surface to the coaptation surface. In the authors’ experience, the need of leaflet resection has been completely abolished even in the case of large excess of tissue.
- Optimal length of neochordae is probably the most controversial issue when considering neochordal repair. Although a large number of methods have been described to achieve an adequate chordae length, basically there are two broad strategies.
- First, the length of neochordae may be predetermined. In these techniques, either pre- or perioperative assessment of length is performed by transoesophageal echocardiogram or by direct measurement using a normal landmark (e.g. neighbouring non-prolapsing segments). The fixed length loop technique is based on the use of a custom-made calliper, and on the distance between the tip of the papillary muscle and the edge of a non-prolapsing segment (usually P1) to determine the correct loop length. In the authors’ opinion, an important anatomical concern regarding this method of measurement should be considered. This reference distance is not fixed due to a great variability in the morphology of the papillary muscles and multiple chordae with different heights can be found in the same valve.
- A second strategy is to leave the length undetermined and adjust neochordae length by testing the valve function. Lengths are adjusted until any regurgitation is eliminated. The required length is obtained by a process of trial and error, and the complexity of this process may increase in case of a large number of neochordae. In the Folding Leaflet technique, the presence of normal leaflet segments as a reference to determine the required chordal length is not necessary. The level of the annulus is used to establish the correct length during the knot tying of the neochord, while the leaflet is folded towards the annulus. This can simplify the procedure in case of complex repairs with the use of multiple artificial chordae.
Summary
In the authors’ opinion, the Folding Leaflet technique facilitates the extensive use of neochordae in the case of large areas of prolapse in both leaflets. This procedure simplifies the adjustment of the length of multiple neochordae, without the need of adjacent healthy chordae or premeasured length by callipers or echocardiography. The long-term durability of this type of repair remains to be seen, but our preliminary experience suggests that it is a safe, reproducible, and effective operation.





Comments