ALERT!
This site is not optimized for Internet Explorer 8 (or older).
Please upgrade to a newer version of Internet Explorer or use an alternate browser such as Chrome or Firefox.
Intern Survival Guide Part 2
Saturday, August 8, 1998
CARDIAC SURGERY
|
||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Anticoagulation | [Table of Contents] |
|
|
|
- Coumadin dosed QAM » No running orders
- INR drawn routinely QPM. Depending on fellow preference and/or the patient's condition, an additional AM INR may be drawn prior to daily dose. Case managers are a useful resource for dose conformation if fellow in O.R.
- Target INR (prior to discharge) for:
Prosthetic aortic valve 2.0 Prosthetic mitral valve 3.0 Paroxysmal Afib 2.0 - 2.5 Novacor LVAD 3.0 - 4.0 (variable) - Elevated INR:
- Notify fellow if INR > 6
- Send repeat INR and T&S
- ****No vitamin K unless approved by fellow!!****
Indiscriminate use of Vitamin K (especially SQ) will result in a lengthy hospital stay as we attempt to re-anticoagulate with coumadin.
- An "anticoagulation sheet" posted on patient's door to be filled in on rounds may help to follow patient's reponse to coumadin
- Usually do not bolus unless late postop or refractory to increases in hourly dose
- Target PTT for all = 1.5 to 2.0 times control
- COUMADIN
- HEPARIN
| Anemia (new onset) | [Table of Contents] |
|
|
|
- Check Hgb (done on ward) and send repeat STAT H8 and T&S
- Is patient symptomatic (orthostatic/fatigued)? Tachycardic?
Can often avoid transfusion if patient asymptomatic » Diuresis will often eventually increase the Hct. - Guiac stools. Initiate ulcer prophylaxis if not currently on it (Zantac IV or Omeprazole PO if thrombocytopenic/altered mental status)
- Consider obtaining CXR to R/O hemothorax or a CT scan to R/O retroperitoneal hematoma in patients with recent femoral catheterization (angiogram, etc.)
- Always check with fellow prior to transfusions! Most attendings consider a Hct of 25 adequate (if patient asymptomatic and revascularized).
| Arrhythmias | [Table of Contents] |
|
|
|
- Occurs in 25 - 30% of cardiac surgery patients » Usually a benign rhythm!
- The fellow should be closely involved in the management of Afib in patients with SBP < 110mmHg especially if no pacing wires in place.
- In these patients, there may be a fine line between rate controlling the Afib and causing marked hypotension.
- Remember synchronized cardioversion (starting levels: 200J for Afib, 20 - 50J for Aflutter) may be necessary if patient hypotensive with:
- Ischemic EKG changes/chest pain
- CHF
- Depressed mental status
- "First do no harm" » If the patient is maintaining an adequte BP without ischemic changes or chest pain, slowing the HR can be done at a slow, safe pace !!! Virtually all revascularized patients can tolerate HRs of 130 - 150 bpm for a significant period of time.
*** The management of patients with low ejection fractions (< 35%) or who are "incompletely revascularized" usually require the close guidance of the fellow for a more expeditious control of the tachyarrhythmia. - Target a HR < 120 bpm. Often when a patient converts to NSR (which occurs spontaneously in 75%!) the HR will be considerably lower.
- Treatment 1: Rate control
(general guidelines » obviously, tailor therapy for each patient):
- Administer the patient's routine PO metoprolol (12.5 - 50 mg) or diltiazem (30 - 90 mg) early or give an extra dose of these agents. In many cases where HR less than 120 bpm, this is all that is necessary
- If this fails or if rate consistently > 120 bpm and the patient has an adequate BP, IV diltiazem boluses (5 - 15 mg each) is usually the treatment of choice. Occasionally, a patient will require a continuous infusion of diltiazem (5 - 15 mg per hr). This infusion can be administered through a peripheral IV, but the patient's monitoring status must be upgraded.
- If the the rate is > 120 bpm and the patient is relatively hypotensive (SBP < 110 mmHg), management should be closely overseen by the fellow. In this setting, IV digoxin and judicious use of IV diltiazem is often successful. Occasionally, synchronized cardioversion is necessary.
- No IV beta blockers should be adminstered unless specifically ordered by the fellow. These agents are infrequently used in the postop cardiac surgery patient.
- Note: Although combining beta-blockers and calcium channel blockers is frequently done on our service, one must be cautious due to potential for refractory AV conduction delays particularly in valve patients). This is especially true once the pacing wires have been removed.
- Treatment 2: Chemical cardioversion
- If Afib is recurrent or persists more than 24 hours, often start procainamide or amiodarone (choice of agent is attending-dependent) »check with fellow. Amiodarone is steadily gaining acceptance in cardiac surgery.
- Procainamide:
- Dosing: Procainamide 1000mg PO (or occasionally IV) then Procan SR 750 - 1000mg Q6hr (in patients with NL renal function)
- Usually have a rate controlling agent on board before starting procainamide » will accelerate conduction through AV node
- Procainamide often causes nausea » Trial of Reglan may be indicated. Persistent nausea may necessitate the discontinuation of procainamide.
- Procainamide can prolong QTc interval and cause torsade de pointes (Treatment: MgSO4 2gm IV over 2 minutes, defibrillation if degenerates to Vfib)!
- Amiodarone:
- Dosing:
PO Load » Amiodarone 600 mg PO BID
or 400 mg PO TID x 5 - 7 daysMaintenance » Amiodarone 200 mg PO QD IV bolus » Amiodarone 150 mg over 10 min IV load » Amiodarone 150 mg bolus followed by infusion of a 900 mg in 500 cc mixture at 1.0 mg/min for 6 hours then 0.5 mg/min for 18 hours - ** Amiodarone has beta-blocking properties » watch heart rate as load and taper other rate controlling agents (beta blockers, calcium channel blockers and digoxin) during load!
- Amiodarone may also increase QTc and cause torsades
- Dosing:
- Anticoagulation:
- If Afib is recurrent or persists more than 6 - 24 hours, usually anticoagulate with heparin because of risk of thrombo- embolism » Check with fellow. (Note: Some attendings prefer to start heparin at the onset of Afib.)
- No bolus in early postop period when initiating herparin drip.
| Pushing IV Calcium Channel Blockers | [Table of Contents] |
- IV administration of calcium channel blockers has almost become a daily activity on the ward. Nevertheless, one must respect the rapid effects that these agents may have on the blood pressure and heart rate » Particularly in elderly patients.
- Currently, IV diltiazem is the agent used most frequently » Primarily due to excellent marketing over the past 5 years. (IV verapamil is also a very good choice and is much cheaper » with time, this agent may be again become the CCB of choice)
- For safe admistration of these agents, follow this checklist:
- Monitor in room (+/- defibrillator), patient in bed, RN available to assist
- Have pacing wires attached to a functioning pacemaker (check battery)
- Have at least one functioning 18 gauge (or greater) IV available (check that it flushes well and painlessly before administering drugs!)
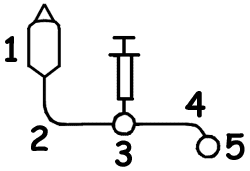
- Have 1 liter NS hanging and connected to IV via primary IV tubing (not through IMED) » see setup. May rapidly need volume if patient becomes hypotensive.
- Have Calcium Chloride stick ready to push
- Will help reverse hypotension caused by diltiazem
- Unless patient crashing, only push a few cc's at a time
- Before you push CaCl, tell patient that they will experience feel a cutaneous flushing sensation
- The fellow should be aware that IV agents are being pushed
|
| VENTRICULAR ARRHYTHMIA | [Table of Contents] |
- Fortunately, an uncommon complication relative to supraventricular tachycardia.
- The most important question is: "How is the patient tolerating the rhythm?"
- If unresponsive/hypotensive, follow ACLS protocol
- If patient alert with satisfactory blood pressure, there is time to determine the origin of the arrhythmia » Not all wide complex tachycardias are ventricular!! More often than not, it is a supraventricular tachycardia with aberrant conduction; however, be aware that a stable BP does not rule out VT.
- The presence of bigeminy/trigeminy does not increase the risk of VT.
- Treatment:
- If unstable, have the fellow and the code team paged as you manage the patient (ACLS protocol). Furthermore, the CSICU should also be notified so that arrangements can be made for rapid transfer to the unit » This is particularly important now that the CSICU is regularly at full capacity.
- Defibrillator and arrest cart in the room; telemetry or defibrillator leads on for in-room evaluation of rhythm
- Obtain/confirm IV access (usually best to have central venous access » femoral catheter may be necessary)
- Bag and mask set up to ventilate if necessary
| AV Conduction Abnormalities | [Table of Contents] |
|
|
|
- Primary AV block (PR interval > 0.2 sec) is relatively common after cardiac surgery.
- It may be due to cold cardioplegic solutions, perivalvular edema or a variety of pharmacologic agents.
- Rarely requires treatment
- If the PR interval is approaching 0.3 sec, hold beta blockers, calcium channel blockers, and digoxin until you check with the fellow.
- Nodal rhythms after valve replacement
- Do not coumadinize until NSR returns. (Why? If after 7 -10 days nodal rhythm persists, permanent pacemaker placed.)
- Symptomatic complete AV block treatment alternatives:
- Pace via operative pacing wires
- Transcutaneous pacing pads
- Isoproterenol drip
- Transvenous pacing catheter
| Chest Pain | [Table of Contents] |
|
|
|
- Obviously, the most important etiology in the differential diagnosis is myocardial ischemia. Fortunately, it is very uncommon in the postop cardiac surgery patient.
- Obtain EKG.
- Compare with preop and early postop EKGs.
- Realize that the EKG may be difficult to interpret due to common changes in repolarization, etc. associated with revascularization and manipulation of the heart / pericardium intraoperatively. Call the fellow to assist.
- Territorial ST elevation is the most concerning finding
- Do not send off CPK curve unless requested by the fellow.
- Most important questions to ask: Did the patient have angina preop? If so, is the pain the same as the pain now?
- Examine patient. Can the pain be reproduced by palpation, positional changes or deep inspiration? If so, much less likely to be ischemic in nature.
- Only give nitroglycerin if after the above rapid assessment, the chest pain is still felt to be myocardial in origin. The fellow should be intimately involved in the management of the patient by this time. As the patient awaits transfer to the CSICU, administer oxygen, nitroglycerin SL and morphine IV as well as cautious use of agents for rate control (if rapid heart rate present). Keep patient on continuous telemetry and stay in the room.
| Chest Tubes | [Table of Contents] |
|
|
|
- Usually pulled prior to transfer from CSICU.
- May be left in and connected to chest tube drainage cannister (i.e. Pleura-vac) if:
- Air leak
- Significant drainage
However, to reduce risk of mediastinitis, most attendings feel that the tubes should be removed by POD 3 or 4. If necessary, new pleural tube(s) can be placed so that the operative tubes can be removed.
- If no air leak, usually put to waterseal the morning following transfer. If no pneumothorax on CXR at 4 hours (confirmed by radiologist or fellow), remove.
- Occasionally the fellow may chose to clamp chest tube (CT) to confirm absence of unsealed parietal pleural defect (simulating removal of chest tube) and obtain CXR in 2 hours. Clamp the CT close to the skin to avoid leaks from tube connections. If no pneumothorax (again confirmed by radiologist), remove.
*** While CT clamped, the patient should be level 4 (or closely monitored by the houseofficer on the floor) and should he/she experience any SOB, chest pain or desaturation »Immediately remove clamp and watch CT drainage cannister for air leak. Put CT to suction again amd obtain STAT portable CXR.
| REMOVAL OF CHEST TUBES | [Table of Contents] |
- Before removing CT, make sure that there is:
- No air leak (If concerned about air leak, consider CXR +/- clamp prior to removal.)
- Minimal drainage over the previous 6 - 12 hours
- Premedicate with Tylox (2 tabs) 45 -60 min prior to CT removal
- If unfamiliar with the technique of chest tube removal, ask the fellow to demonstrate it.
- Assorted points to remember:
- Never pull CT before 7:30 AM or after 5 PM (if after 3 PM, notify the fellow). Fatal hemorrhage has occurred with bypass conduits avulsion at the time of CT removal » If done during "working hours", an O.R. team can be quickly assembled.
- Once starting to pull CT, don't hesitate even if feel resistance » A common cause of pneumothorax is a pause in mid- pull with the patient inspiring through a side hole of the half- removed CT.
- Post-removal CXR should be portable » The patient should be monitored for complications (pneumothorax, bleeding, etc.)
- Pneumothorax (PTX) after removal of CT:
- Some PTX may be observed and allowed to resorb
- As a general rule, if the PTX extends more than halfway down the lateral chest wall or is more than 2 cm down at the apex, a small (20 Fr) CT is necessary. (This is particularly true in our patient population with significant tobacco abuse history and marginal pulmonary reserve.)
- If the patient is clinically stable and in no respiratory distress, placement of the CT is not emergent. Have a chest tube insertion set and chest tube in the room. Obtain consent for procedure. Check current coagulation studies (+/- have T&S available for possible FFP). The fellow will place CT or assist you in placing CT once he is available.
- If the patient is in respiratory distress, notify the fellow (or if not immediately available, the senior surgical resident in the CSICU) for urgent CT placement. Consider emergent decompression with 14 gauge IV (ICS 2 midclavicular line) until they arrive if patient is rapidly decompensating !!
- Supplies for chest tube insertion:
- Chest tube insertion kit (instruments and prep set)
- Chest tube (20 - 24Fr for pneumothorax, 28 - 32Fr for effusion)
- Chest tube drainage cannister (Pleura-vac, etc.) and 250 cc saline
- Xylocaine (1% or 2%) 50 cc vial
- Extra #0 or #1 Vicryl (from O.R.)
- Betadine
- Xeroform sheet
- Chucks (disposable absorbant sheets)
- IV Morphine
- Monitor
| Chest X-rays | [Table of Contents] |
|
|
|
- Routine CXR performed on POD 3
- "Routine" postoperative findings include:
- Mild-moderate L effusion
- LLL atelectasis
- Look for the following significant findings:
- Large (or increasing) L effusion
- Infiltrate
- Pneumothorax
- CHF (some degree of pulmonary edema is NL until postoperative diuresis complete)
- Increasing cardiac silhoutte (?pericardial effusion)
- Elevation of hemidiaphragm (?phrenic N. injury)
- Retained foreign body (sponges,etc.)
| CPR | [Table of Contents] |
|
|
|
- Be certain that the patient truly is pulseless before initiating chest compressions ! Effective compressions usually result in sternal fractures in our elderly population. Many post-op cardiac surgery patients who require CPR will need debridement of sternum and pectoralis muscle flaps due to sternal instability.
- Slide chest compression board under patient's back
- Place towel over median sternotomy staple line to avoid cutting palms during CPR
Table of Contents | CTSNet HOME | RESIDENTS' Section | NEXT Page
| The author has taken care to make certain that the treatment regimens and drug doses are correct and compatible with standards of care accepted at the time of publication. Changes in treatment or drug dosage become necessary as new information becomes available. Consult package insert for drugs before administration. |