ABSTRACT
Ten-year old child presented with recurrent hemoptysis and a bout of massive hemoptysis. Chest radiography and computerized tomography revealed a soft tissue mass in the right lower lobe. Emergency right lower lobectomy revealed echinococcal cyst as the cause of the exsanguinating bleed.
PRESENTATION
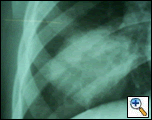
In the evening of July 1, 2005 a ten-year old child was brought to the emergency wing of the Government Medical College, Hospital Jammu in north India with history of two bouts of hemoptysis (each of 200 to 300 mls) on the morning of admission. He initially coughed out dark clotted blood, followed by frothy bright red blood. Examination revealed pallor and bronchial breathing & crepitance in the right infrascapular area. A previous chest x-ray in May 2005 (CXR Figure 1) and contrast enhanced computed tomography chest (CECT, Figure 2) revealed a variegated soft tissue mass in the right lower lobe.
 |
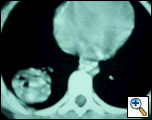 |
| Figure 1: Rounded radio opacity in right lower lobe. | Figure 2: Well defined mass in right lower lobe having variegated soft tissue attenuation. A few small air pockets seen in the center of the mass. |
The patient had a significant past history of pleuritic pain in the right lower chest in June 2004. This responded to analgesic and antibiotic treatment for four days and no further investigation was carried out at that time. There was no history suggestive of trauma, tuberculosis or congenital heart disease. However, the patient did have a history of contact with a pet dog and sheep.
He remained asymptomatic until January 2005, when he developed high-grade fever (103oF) followed by productive cough with yellow-colored sputum (the sputum was negative for tubercle bacicilli). The following day, he developed hemoptysis – clotted dark red blood followed by bright red blood mixed with the sputum. At that time, he was admitted to the pediatric department of our Hospital. Ultrasonography revealed a normal liver and small amount of right pleural effusion.
Laboratory data revealed total leukocyte count of 11,900/mm3 with 69% polymorphs, 28% lymphocyte, and 3% eosinophils and a hemoglobin of 11.2 g%. Once again, he was treated successfully with antibiotics and his symptoms abated within a week.
During the night of his current admission (July 1, 2005), he developed a massive hemoptysis of 1.5 liters. Following resuscitation, the patient was taken for an emergency right lower lobectomy. The right lower lobe was adherent to the diaphragm and the posterolateral parietal pleura.
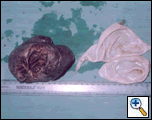
On making an incision on the resected specimen from posterolateral aspect, a collapsed white lamellar membrane peeped out. Macroscopic examination (Figures 3 & 4) revealed a cavity (6.5x5.5x5 cms) outside the lamellar membrane, which had a soft clot leading to a peripheral pulmonary artery. Adjacent & posterior to the opening of the peripheral pulmonary artery were two openings of branch bronchi. Biopsy confirmed hydatid cyst as the cause.
 |
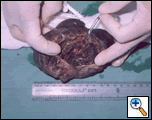 |
| Figure 3: Cut Specimen along with lamellar membrane. | Figure 4: Specimen with canulated branch bronchi and branch pulmonary artery opening into the cavity. |
He had an uneventful post-operative recovery. He was put on intravenous ceftriaxone, amikacin, and tinidazole for three days followed by oral cefixime and intramuscular amikacin for four additional days. He was discharged on the fifth postoperative day.
DISCUSSION
Hydatid cyst is a rare cause of hemoptysis in children. Common causes of pediatric hemoptysis include infection, foreign body aspiration, tracheostomy-related problems, congenital heart disease, cystic fibrosis, pulmonary hemosiderosis, trauma, and fictitious hemoptysis [1].
Cough, chest pain, and breathlessness are the most common presenting symptoms. While hemoptysis is a presenting symptom in adult patients in up to 70%, it is a rare presentation in pediatric patients. Bharati et al have reported a six-year old child who presented with two episodes of small quantity (5 to 10 ml) hemoptysis with the diagnosis of pulmonary hyatid cyst in the left upper and lower lobes in addition to four cysts in the right lobe of the liver [2]. The incidence of hemoptysis in children may be as high as 38% in one a series by Solak et al [3].
The mechanism of hemoptysis in pulmonary hyatid disease may be due to pressure erosion of a bronchus or obstructive effect with bronchial infection. This may in turn lead to further erosion into a branch arterial supply leading to hemopytysis. Hydatid cysts not only may erode into bronchi, but also vascular structures including the aorta causing massive hemoptysis [4]. It is possible that during bronchoscopy, the cyst can perforate causing hemoptysis [5].
The principles of surgical management of a pulmonary hydatid disease include the complete evacuation of the cyst with elimination of the endocyst and the avoidance of contamination and management of residual cavity. Normal lung parenchyma must be preserved as much as possible. For cysts with abscesses or severe pulmonary destruction, segmentectomy, lobectomy, or even pneumonectomy are required. Video-assisted thoracoscopic surgery is contraindicated in huge thoracic cysts secondary to the risk of hypersensitive reaction, asphyxia, and recurrence due to cyst rupture [6]. Rebhandl et al reported two recurrences after a mean follow up of 4.8 years in a series of 33 children with 49 pulmonary hydatid cysts who underwent surgery. They concluded that the therapy of choice in pediatric pulmonary hydatidosis is complete surgical elimination of cyst by cystotomy and capitonnage and ideally benzimidazole treatment should be combined with surgery [7]. Celik and his colleagues believe that lung parenchymal preservation procedures without capitonnage is preferable [8].
In order to distinguish the role of medical versus surgical treatment in childhood hydatidosis, Keramidas et al studied the anatomical site of the disease as well as type and results of treatment in 146 echinococcosis cases [9]. They concluded that medical management of pediatric pulmonary hydatid disease is generally effective in 4% [9]. About one third of patients on medical treatment developed complications requiring surgical intervention.
More recently, Keramidas et al treated 36 children with pulmonary Echinococcus cysticus with oral mebendazole or albendazole. During this treatment, 11 patients developed complications requiring surgical intervention. In all cases that developed complications, the mean size of the cysts exceeded 6 cm in diameter at the initiation of medical treatment. They concluded that a) large pulmonary hydatid cysts should not be treated medically, b) incomplete expectoration of the cyst contents after the parasite death may lead to infection through bronchial communication, and c) patients surgically treated for complications following medical treatment are hospitalized twice as long as patients surgically treated in the first place [10].
In our patient, it appears that the echinococcal cyst had initially caused obstruction to the branch bronchi leading to stasis. This lead to an infection resulting in transmigration of bacteria to right basal pleura causing localized pleuritis. During the following six months, the cyst may have eroded the branch bronchi and peripheral pulmonary artery causing recurrent hemoptysis and later massive hemoptysis. Emergency right lower lobectomy was performed to prevent the exsanguinations.
References
- Batra PS, Holinger LD. Etiology and management of pediatric hemoptysis. Ann Otolayngol Head Neck Surg 2001;127:377-382.
- Sahul B, Bhavneet B. Hydatid disease of lungs – unusual cause of hemoptysis. Indian Pediatrics 2002;39:1062-1063.
- Solak H, Yenitzeri M, Yuksek T, Anil N, Goktogan T, Ceran S. The hydatid cyst of lung in children and results of surgical treatment. Thorac Cardiovasc Surg 1990;38:45-47.
- Harris DG, Van Vuuren WM, Augustyn J, Rossouw GJ. Hydatid cyst fistula into the aorta presenting with massive hemoptysis: case report and literature review. J Cardiovasc Surg (Torino) 2001;42:565-7.
- Toker A, Tanju S, Bayrak Y, et al. Life threatening hemoptysis in a child; the only symptom. Ann Thorac Surg 2004;77:336-8.
- WU M, Zhang L-W, Zhu H, Qian Z-X. Surgical treatment for thoracic hydatidosis: review of 1230 cases. Chinese Medical J 2005;118:1665-1667.
- Rebhandl W, Turnbull J, Felberbaur FX, et al. Pulmonary echinococcosis (hydatidosis) in children: results of surgical treatment. Pediatr Pulmonol 1999;27:336-340.
- Celik M, Senol C, Keles M, et al. Surgical treatment of pulmonary hydatid disease in children: report of 122 cases. J Pediatr Surg 2000;35:1710-3.
- Keramidas DC, Passalides AG, Soutis M, Antoniou D. Hydatidosis management in children: does anatomical location affect type of treatment?. International association of hydatology, Newsletter of the Hidatidosis, 1997 Is. 15.
- Keramidas D, Mavridis G, Soutis M, and Passalidis A. Medical treatment of pulmonary hydatidosis: complications and surgical management. Pediatr Surg Int 2004;19: 774-776 Epub 2004 Jan 9.




