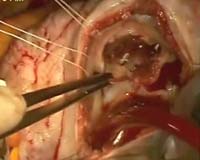
This video describes the cone procedure for tricuspid valve repair in a 35-year old NYHA class II patient with Ebstein anomaly presenting with reduced exercise tolerance and episodes of paroxysmal atrial fibrillation.
Echocardiography and MRI confirmed the diagnosis of Ebstein anomaly, with severe downward displacement of the posterior and septal leaflets, torrential regurgitation and a moderate size ASD.
The fundamental principle of the cone repair is mobilization of the anterior and posterior tricuspid valve leaflets from their anomalous attachments in the right ventricle, and the clockwise rotation of the free edge of this complex to be sutured to the septal border of the anterior leaflet. This creates a cone the vertex of which remains fixed at the right ventricular apex and the base of which is sutured to the true tricuspid valve annulus level.
On the operating table, normothermic cardiopulmonary bypass (CPB) was established and antegrade cold blood cardioplegia used for myocardial protection. After opening the right atrium, several stay sutures were placed in the valve annulus for exposure and for marking the area were the new true annulus had to be reconstructed. Examination of the valve leaflets confirmed the diagnosis of severe Ebstein anomaly. The anterior leaflet was partly detached from the annulus and the resection carried out posteriorly to completely detach the posterior leaflet from the right ventricle. Aggressive muscle resection was performed underneath the leaflet taking care not to injure the papillary muscle. This allows complete freeing of the posterior leaflet from its muscular attachment and provides enough tissue to reattach into the new true annulus after creating the cone geometry. Plication of the atrialised portion of the right ventricle was then performed trying to reduce the annular size as much as possible (=ring size 30-32). The posterior leaflet was then reattached into the new true annulus using a double 4-0 Prolene suture line, taking care at the level of the septal portion of the annulus to avoid the conduction system. In this particular case the septal leaflet was left in situ being very small, completely attached to the ventricular wall, and without any subvalvular apparatus. The procedure was then completed and the valve was fully competent on the water test.
The ASD and right atrium were closed, the cross clamp released, and sinus rhythm restored. The patient was weaned from CPB in satisfactory haemodynamic state. Echocardiography confirmed a well-functioning tricuspid valve, with significantly reduced right side dimensions and good biventricular function. The patient made an uneventful recovery and was discharged home 7 days post-operatively.
The cone procedure is an effective and reproducible technique for tricuspid valve repair in Ebstein anomaly and has been adopted in our Unit as the first choice surgical strategy in this very high-risk group of patients.
Acknowledgment
The authors are very grateful to Dr Mark Hamilton for providing the MRI and Echocardiographic pictures.
Video:




