ALERT!
This site is not optimized for Internet Explorer 8 (or older).
Please upgrade to a newer version of Internet Explorer or use an alternate browser such as Chrome or Firefox.
Minimally Invasive Approach to Pancoast Tumor Using 3D Printing
Case Presentation
The patient was a 64-year-old woman with a 20 pack-year smoking history. She presented with vague right upper extremity pain, which was diagnosed as a right superior sulcus tumor. The patient was reviewed by the multidisciplinary thoracic tumor board and determined to be an excellent candidate for neoadjuvant therapy. She completed two cycles of concurrent cisplatin with etoposide and received 4,500 cGy of radiation. She recovered well and was re-staged at four weeks. Repeat imaging confirmed tumor response to treatment, as well as resectability of the tumor. However, scans revealed possible involvement of the T1 nerve root and the first and second ribs. Three-dimensional (3D) modeling was used in pre-operative multi-specialty planning, and in patient education. The patient was taken to the OR and, as demonstrated in the video, underwent a thoracoscopic lobectomy with limited para-scapular incision for management of the T1 nerve root and removal of the specimen. The latissimus and serratus were spared, and no rib-spreading was required to complete the surgery. The patient was ambulatory the morning after surgery and began rehabilitation. She had excellent pain control throughout recovery. Although she did have expected sensory deficits from her T1 nerve root sacrifice, her muscular manifestations were minimal. She was doing very well at the time of follow-up.
Technical Aspects of 3D Printing
The Mayo Clinic, Rochester, Minnesota, has utilized three-dimensional models since 2006. More than 130 models have been created for a variety of surgical specialties and pathologies (Figure 1).
Three dimensional modeling begins with the acquisition of two-dimensional images in DICOM format: an X-ray, CT scan, or an MRI. A series of slices, or a “stack,” of two-dimensional images of a particular anatomical structure are used to create the model. Each structure of interest is segmented by a technician. Depending on the size, resolution, and complexity of the structure, proprietary software or manual tracing are performed at sequential levels to generate a three-dimensional volume that can be converted into a mathematical surface. The surface geometry is written into a stereolithography (STL) file format, which can be sent to the 3D printer (Stratasys Connex 350 polyjet; Figures 2 and 3). A model is created using liquid polymers that are laid down onto the surface and then exposed to UV light to solidify prior to the next layer application.
 |
 |
 |
| Figure 1: Example of the three-dimensional models used in pre-operative planning. |
Figure 2: Stratasys Connex 350 Polyject Printer. |
Figure 3: Stratasys Connex 350 Polyjet Printer, close view. |
Operative Considerations and Benefits
Planning for complex surgical resections can be somewhat limited when forced to rely solely on two-dimensional imaging. Three-dimensional (3D) printed models using imaging from high resolution CT scanning provide a better understanding of complex anatomical relationships, thereby allowing more thorough pre-operative planning. This becomes particularly pertinent when developing a multi-specialty operative intervention. The models allow surgeons the opportunity to rehearse the procedure, select appropriate instrumentation, and divide task responsibility, while anticipating potential obstacles prior to the patient entering the operating theater.
An educational benefit is seen both in pre-operative patient and family counseling, as well as with resident education. The model can be used to teach potential anatomic abnormalities, predict hazards, demonstrate important adjacent structures, and simulate anatomy. A further use of 3D printing is in the creation of anatomical scaffolds for the creation of grafts and implants. These features were not used in this particular case.
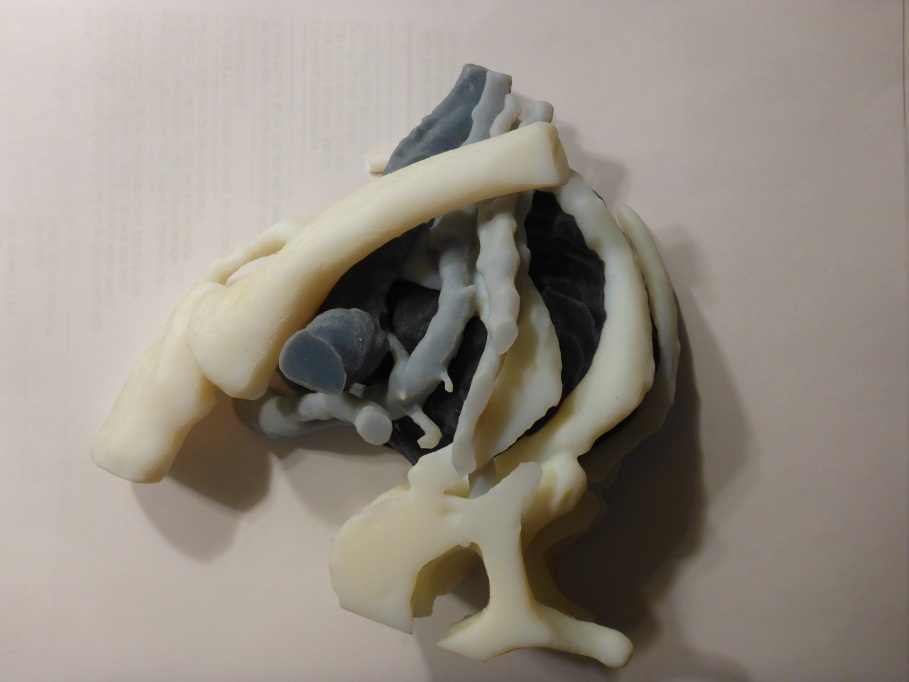
This case highlights the benefits of 3D models. A 3D model was created and reviewed with the patient and her family (Figure 4). She had the opportunity to see the relationship of her tumor to her ribs, spine, and the involvement of her T1 nerve root. She developed a much more thorough understanding of the surgical plan, including the necessity of sacrificing the T1 nerve root, as well as other operative challenges and risks.
The anatomic model was used in conference with the orthopedic spine surgeons to discuss the potential approaches to resection of the mass. A minimally invasive approach to the lobectomy, with limited posterior incision to access the T1 nerve root, was deemed possible because of the 3D modeling.
Pre-operatively, the team was able to select port placement, practice the approach to hilar structures, and determine the required stapler angles to perform the lobectomy from an anterior-only approach with the obstacle of the adherent tumor to the chest wall (Figure 5). Furthermore, the team was able to prepare for the possibility of rib resection using minimally invasive spine instrumentation.
At the time of surgery, the lobectomy and chest wall resection were approached as practiced on the 3D model. The hilum was handled as planned. The vein, arterial branches, and bronchus were skeletonized and divided with staplers. Involvement of the pleura was easily visualized by the thoracoscopic approach. An extra-pleural dissection was initiated at the level of the 4th rib and carried cephalad. The second rib was confirmed to be densely adherent to the tumor and an en bloc resection was felt to be necessary for this portion of the chest wall. A Kerrison bone cutter and a Midas Rex diamond bur were selected and tested during the pre-operative 3D planning process to divide the first and second ribs.
An adjunct posterior incision was created along the lateral border of the scapula to allow access to the T1 nerve root. Due to careful pre-operative planning and a minimally invasive approach to the lobectomy, only an accessory para-scapular incision was required to allow for the disarticulation of the first and second ribs and the sacrifice of the T1 nerve root. With this approach, the latissimus and serratus muscles were spared and no rib-spreading was required. The thoracoscope was used throughout to facilitate a safe dissection around the subclavian vessels and brachial plexus, and to guide anterior division of the first and second ribs.
The 3D modeling enabled the delivery of a safe and efficient surgery with limited postoperative discomfort and an accelerated recovery.
 |
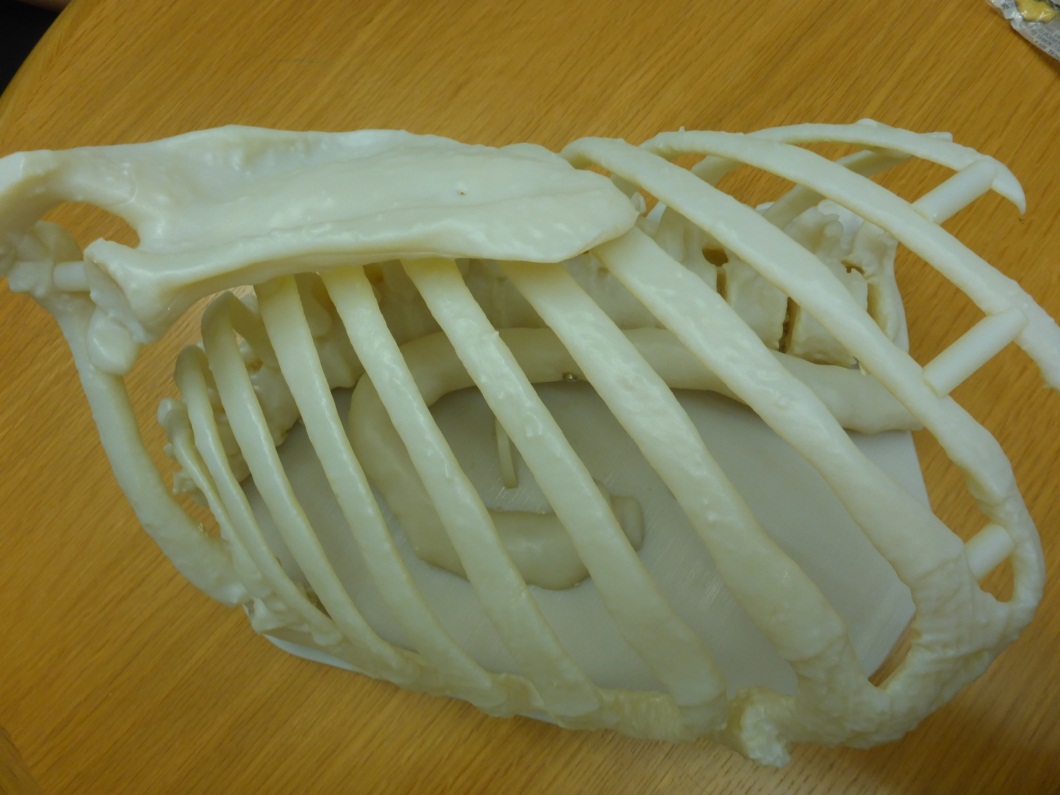 |
| Figure 4: Three dimensional model of superior sulcus tumor with involvement of T1 nerve root. | Figure 5: 3D printed thoracic model to rehearse surgical approach to tumors. |
Time and Cost
The time required to create a 3D model varies with the complexity and size of the anatomic structures selected. Technicians must first create an STL file, which is then sent to the printer. The creation of the model may take anywhere from hours to days to complete. Adequate time must be reserved.
Certainly, cost should always be considered when introducing new technology into a program. The average cost of a 3D printer for the creation of anatomic models is US $200,000. However, after the initial purchase, cost is limited to the materials used to create the model and maintenance. The size, complexity, and printing material will all impact the cost of each model, which can range from a few hundred to a few thousand dollars. With advances in technology and more prevalent usage of the 3D printing, there will likely be reductions in cost.
Summary
3D printing is becoming more widely used in medicine, particularly in the preparation for complex cases. The technology facilitates multi-disciplinary pre-operative surgical planning, assists in the navigation of complex or obscured anatomical relationships, and allows surgeons to rehearse surgical approaches on models prior to taking the patient to the operating room. This technique may enhance a more rapid progression to more advanced surgery by allowing surgeons to practice and think about their cases with life-sized models that are a virtual simulation of the case they have to plan. The model proved to be invaluable in this novel first-reported hybrid-minimally invasive approach to a large superior sulcus tumor.





Comments