ALERT!
This site is not optimized for Internet Explorer 8 (or older).
Please upgrade to a newer version of Internet Explorer or use an alternate browser such as Chrome or Firefox.
Redo Tracheal Resection and Laryngotracheal Reconstruction for Recurrent Subglottic Cicatricial Stenosis
A 19-year-old male was referred to the authors’ department from another hospital because of a tight recurrent subglottic stenosis following tracheal resection and reconstruction for subglottic post-intubation stenosis. Several rigid bronchoscopies had already been performed without any effective result. The patient presented with left vocal cord palsy, probably due to previous treatments.
On admission, a rigid bronchoscopy was attempted to dilate the stenosis by laser-assisted mechanical resection. Due to the extent and hardness of the lesion no effective dilation was obtained, preventing placement of a Dumon stent or Montgomery tube.
Following orotracheal intubation with a 5.0 mm tube, the patient underwent redo cervicotomy, as normal subplatysmal anatomy had been modified by previous surgical approaches, a tracheal stoma, and a severe inflammatory reaction. Dissection was carried out along the surface and border of the sternocleidomastoid muscles on either side. Initial dissection was carried up to the level of the cricoid cartilage; inferiorly, cutaneous and platysmal flaps were raised to the sternal notch. The medial margins of the sternohyoid muscles were identified and elevated laterally for a short distance, followed by the sternothyroid muscles. The anterior surface of the trachea was then dissected.
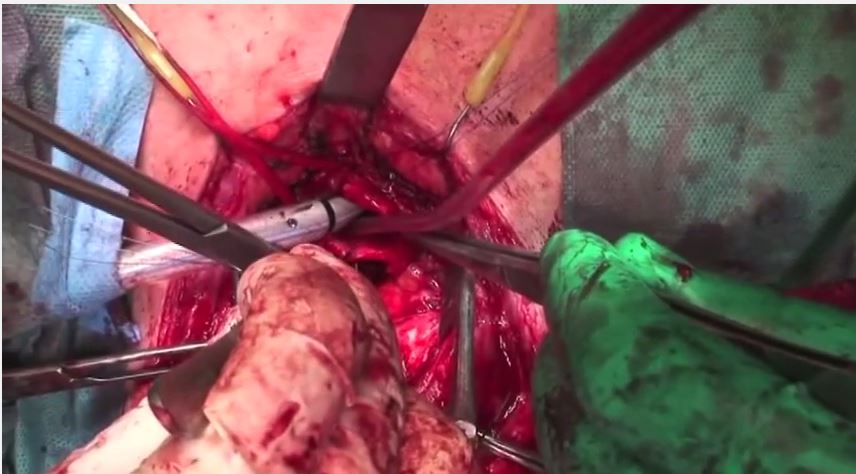
The thyroid was dissected away from the tracheal wall on either side; the substernal plane was bluntly dissected to maximize tracheal mobilization, but without the need for sternal or manubrium division. In the area of stenosis, dissection was kept very close to the scarred portion of the trachea to avoid damaging the recurrent laryngeal nerves. Circumferential dissection of the trachea was performed only at the level of the stenosis, and for no more than 1 to 2 cm above and below that level, to avoid injury to the blood supply that could result in subsequent tracheal necrosis and severe restenosis.
Once the tracheal stenosis was completely isolated, the anesthetist was asked to deflate the cuff on the endotracheal tube. A flexible endotracheal tube with its connectors and sterile anesthesia tubing were clipped into place at the level of the incision, and the proximal anesthesia tubes were passed through the drapes to the anesthetist. The trachea was then divided transversely. The distal trachea was intubated across the operative field, inflating the cuff just enough to obtain a seal. Dissection was completed in areas of difficult scarring until the proximal end of the area of stenosis was reached. Great care was taken proximally when approaching the cricoid cartilage with its severe inflammatory reaction.
Following complete excision of the stenotic tracheal tract, the patient’s neck was put in flexion with the chin approaching the upper sternum. An anastomosis with interrupted 4-0 PDS stitches was commenced with an initial suture posteriorly in the midline of the membranous wall, which passed from outside into the lumen, in either the upper or the lower segment of the trachea, and then from inside to outside in the opposite segment. Sutures were placed approximately 4 mm apart and 3 to 4 mm away from the cut edge of the trachea. When all posterior anastomotic sutures were placed, the endotracheal tube across the field was removed. The orotracheal tube was drawn into the field and positioned beyond the anastomosis, and a guiding catheter was then removed. The anterior defect was sutured. A leak test was performed.
A suction drain was placed in the pretracheal space, and strap muscles were sutured in the midline. The platysma was closed and the skin sutured with subcuticular stitches. Two heavy “guardian” sutures were placed to prevent excessive extension of the neck in the immediate postoperative period. This suture passed transversely through a generous bit of skin in the submental crease and then through the presternal skin. Postoperative flexible bronchscopy confirmed the full patency of the anastomosis.
The patient’s postoperative course was uneventful and he was discharged on postoperative day 14.




