ALERT!
This site is not optimized for Internet Explorer 8 (or older).
Please upgrade to a newer version of Internet Explorer or use an alternate browser such as Chrome or Firefox.
Single-Incision VATS (SIVATS) Segmentectomy for Lung Cancer
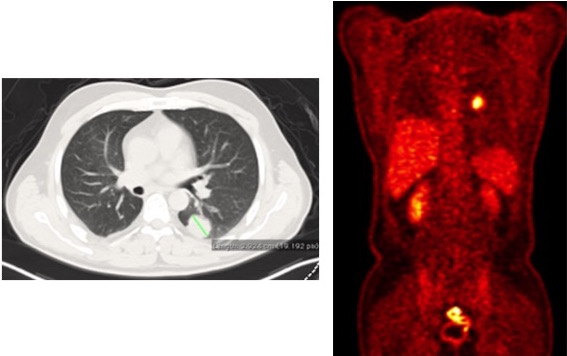
A 49-year-old male patient was operated on by the authors for a T4 (left atrium invasion) squamous cell carcinoma in the right lower lobe (Figure 1). pTNM was T4N0MO and four cycles of chemotherapy were given as adjuvant therapy. After four years of follow-up care, a chest CT showed a newly developed tumor (2.9cm) in the superior segment of the left lower lobe (Figure 2). Since there was no other increased FDG uptake in another part of the body, resection of the tumor was recommended by the Tumor Board.
The authors reserve segmental resections for lung cancer treatment in patients with limited pulmonary functions, resection of metastasis, or small-sized second primary lung cancer with no lymph node metastasis. Intraoperative frozen section pathology is performed at every step of the segmentectomy operation to avoid an incomplete oncological surgery. If appropriate in terms of the intraoperative findings and frozen section pathological analyses, the authors planned to perform a single-incision VATS (SIVATS) superior segmentectomy of the left lower lobe.
SIVATS remains a feasible approach in anatomical lung resections including lobectomy, pneumonectomy, and segmentectomy. With its single intercostal entrance feature, SIVATS seems advantageous over not only thoracotomy but also over standard 3-port VATS and robotic operations. However, further comparative analyses of different approaches remain necessary for a scientific conclusion.
Are you using a mobile device? Download the CTSNet Videos app and watch CTSNet videos conveniently, on the go.






Comments