ALERT!
This site is not optimized for Internet Explorer 8 (or older).
Please upgrade to a newer version of Internet Explorer or use an alternate browser such as Chrome or Firefox.
Unusual Presentation of an Inflammatory Myofibroblastic Tumor
Abu Asbeh, Yousef; Naroditsky, Inna; Katz, Amit; Haberfeld, Ori; Orlovsky, Michael; Kremer, Ran (2017): Unusual Presentation of an Inflammatory Myofibroblastic Tumor.
CTSNet, Inc.. https://doi.org/10.25373/ctsnet.5233969
Retrieved: 19:30, Jul 21, 2017 (GMT)
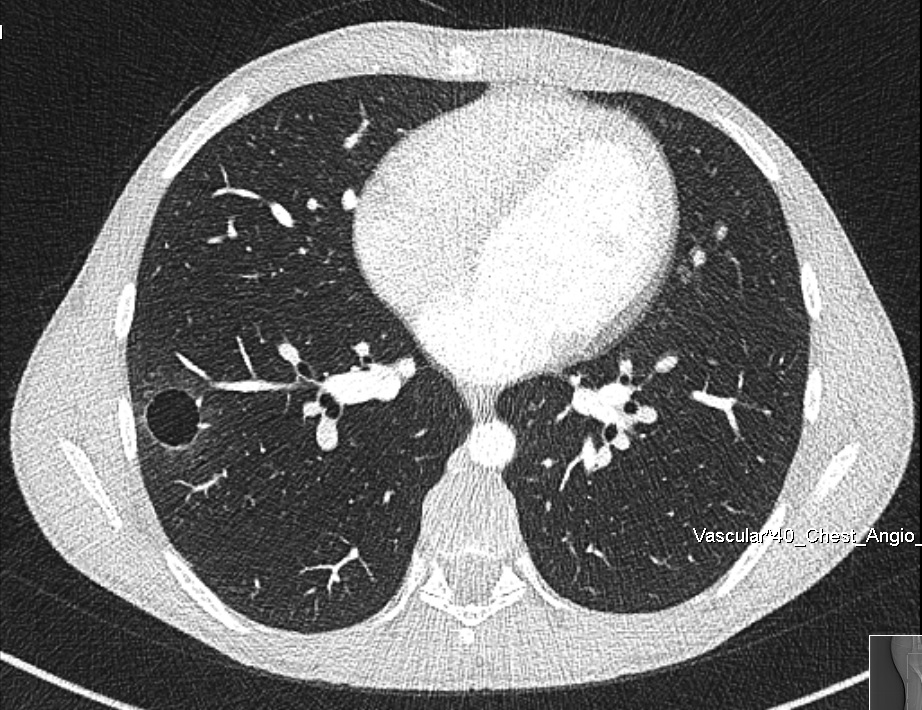
Figure 1. Chest CT scan.
Abstract
Inflammatory myofibroblastic tumors (IMT) are relatively benign tumors that can occur in the lung, and also arise from different anatomical locations. In the lung, an IMT can be a solitary pulmonary nodule or a locally invasive lesion. The authors share the case of a 15-year-old male patient who presented with occasional hemoptysis. A chest computed tomography (CT) scan showed a cavitary lesion in the right lower lung lobe. A thoracoscopic segmental resection was performed, and the pathological result was an IMT. To the best of the authors’ knowledge, there are very limited reports of a lung IMT presenting as a cavitary lesion in the English literature.
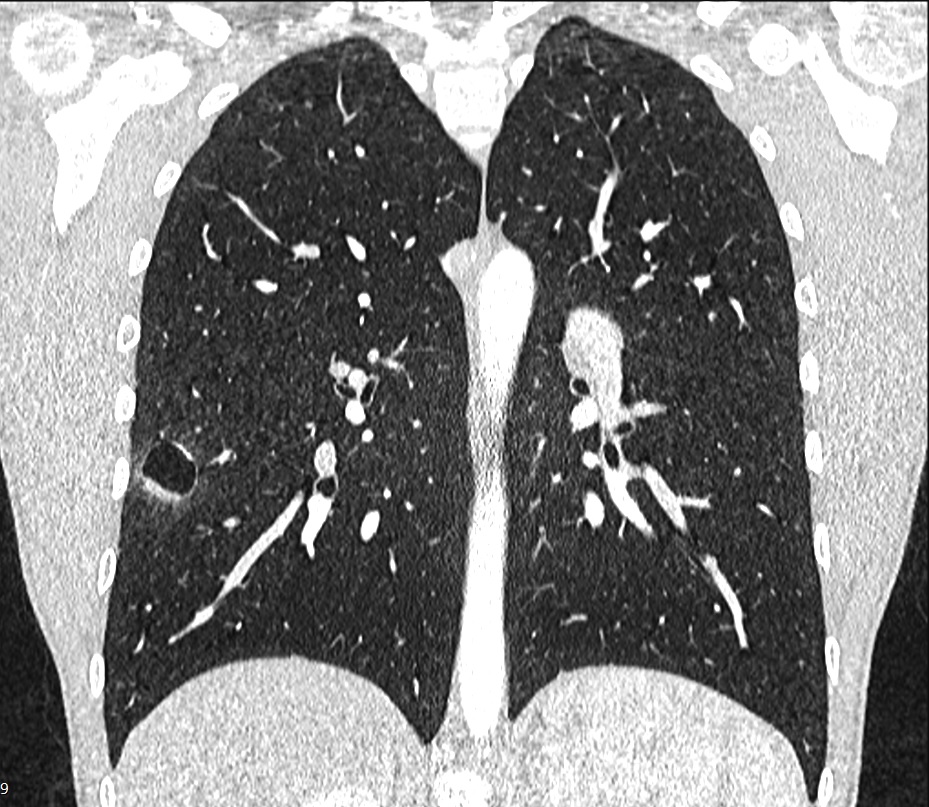
Figure 2. Cavitary lesion in the right basomedial segment.
Background
Inflammatory myofibroblastic tumors (IMT) were first observed and described by Bunn in 1939, and were later named by Umiker and colleagues. IMTs are a rare type of lesion that affect different anatomical locations of the body, and they make up 0.7% of tumors in the lung, parenchyma, and bronchus (1). An IMT usually presents as a solitary nodule but can also present as a locally invasive lesion. Pathologically, IMTs are identified by a proliferation of spindle cells associated with a variably dense polymorphic infiltration of mononuclear inflammatory cells.
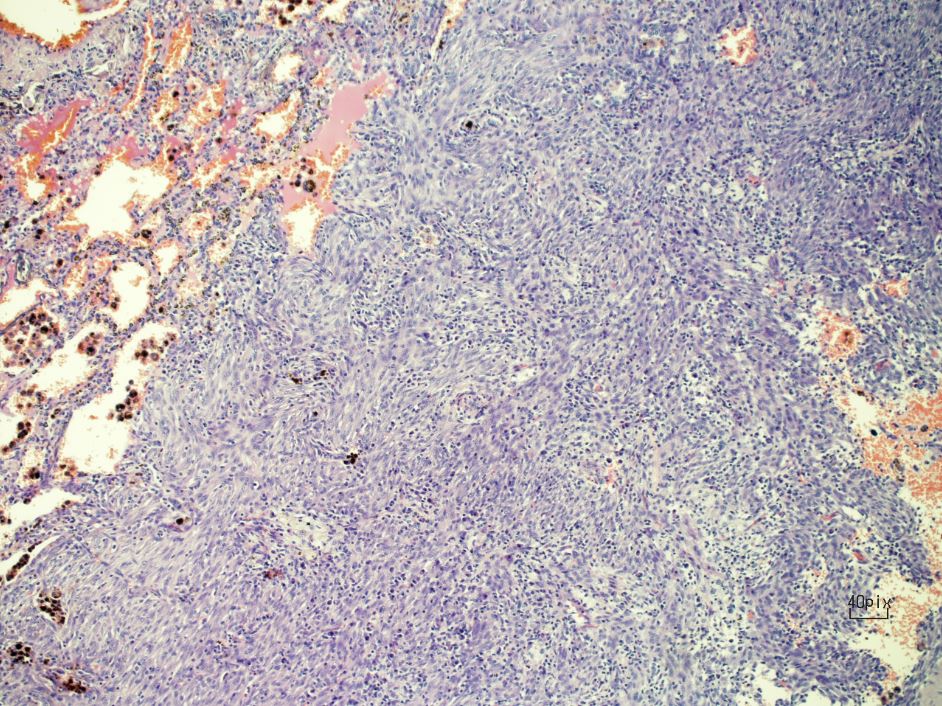
Figure 3. Bland-looking spindle cells.
IMTs tends to occur in individuals under 40 years of age, with both sexes affected equally (2). The most common clinical presentation is asymptomatic, but IMTs can present as dyspnea, cough, chest pain, or hemoptysis. Radiologically, an IMT typically presents as a solitary, peripheral, sharply circumscribed mass with a predilection for the lower lobes. Local invasion and primary involvement of the mediastinum and hilar structures are unusual manifestations (3).
The authors report on the case of a 15-year-old male patient who presented with a two-year history of recurrent hemoptysis (about 60 ml), occurring once every three to four weeks. The hemoptysis was not related to physical activity or other respiratory symptoms and was self-limiting. The patient underwent a diagnostic fiber optic bronchoscopy that was inconclusive. A chest CT scan showed a cavitary lesion in the right basomedial segment of the right lower lobe of the lung. The patient's case was discussed in a multidisciplinary board meeting, and it was agreed that the right lower lobe lung lesion was the most probable cause of the patient's condition. The team planned a thoracoscopic uniportal video-assisted segmental resection of the right basomedial segment of the right lower lobe. The operative course was uneventful. The chest tube was removed three hours after the surgery, and the patient was discharged home on postoperative day one.
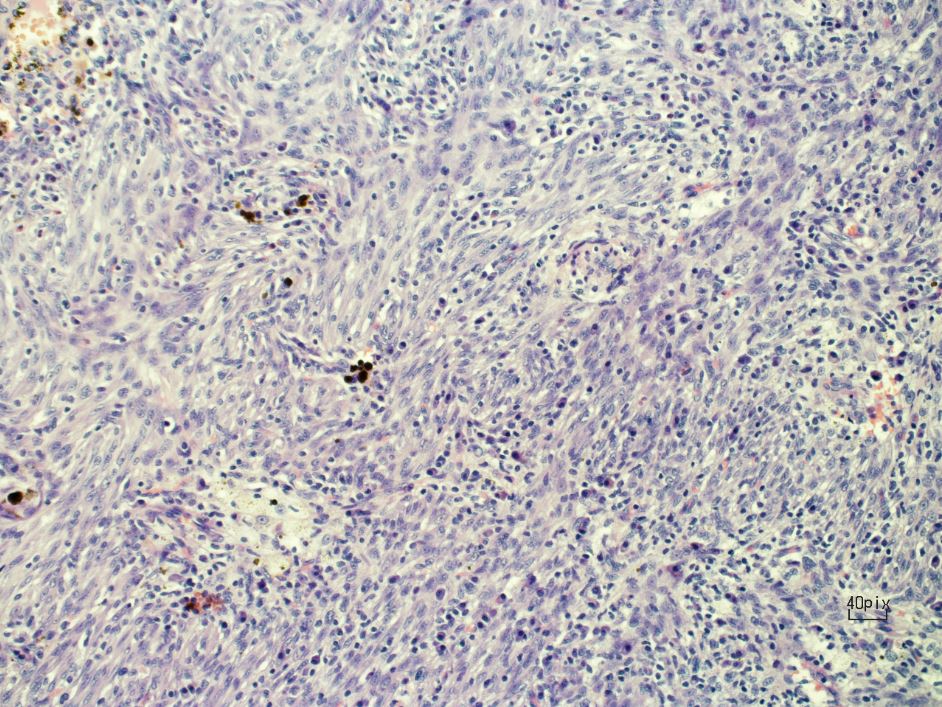
Figure 4. Spindle cells, plasma cells, lymphocytes, foamy macrophages, and hemosiderin-laden macrophages.
The biopsy specimens from the lesion showed IMTs. The patient was free of symptoms at the two month follow-up exam.
Comment
The characteristic radiological presentation of IMTs is usually a peripheral, solitarily, sharply circumscribed lobulated mass. These lesions can be located in the parenchyma (85.7% of cases), endobronchial (10.7% of cases), and endotracheal in (3.6% of cases) (3). To the best of the authors’ knowledge, there are a very limited number of reported IMT cases with cavitary presentation. The authors will continue to monitor the patient annually for recurrence of the IMT or hemoptysis symptoms.

Figure 5. Spindle cells diffusely positive for ALK1.
References
- Golbert ZV, Pletnev SD. On pulmonary pseudotumours. Neoplasma. 1967;14(2):189-198.
- Demirhan O, Ozkara S, Yaman M, Kaynak K. A rare benign tumour of the lung: Inflammatory myofibroblastic tumour-case report. Resp Med Case Rep. 2013;8:32-35.
- Agrons GA, Rosado-de-Christenson ML, Kirejczyk WM, Conran RM, Stocker JT. Pulmonary inflammatory pseudotumor: radiologic features. Radiology. 1998 Feb;206(2):511-518.
- Pinillaa I, Herreroa Y, Torresa MI, Nistalb M, Pardoa M: Tumor inflamatorio miofibroblástico pulmonary. Radiologa. 2007;49:53-55.
- Zhang Y, Dong ZJ, Zhi XY, Liu L, Hu M. Inflammatory myofibroblastic tumor in lung with osteopulmonary arthropathy. Chin Med J (Engl). 2009;122(24):3094-3096.
- Racil H, Saad S, Ben Amar J, Cheikh Rouhou S, Chaouch N, Zarrouk M, Chabbou A. Pseudotumeur inflammatoire pulmonaire invasive. Revu Méd Interne. 2011;32:e55-e58.




