ALERT!
This site is not optimized for Internet Explorer 8 (or older).
Please upgrade to a newer version of Internet Explorer or use an alternate browser such as Chrome or Firefox.
Stent Placement and Catheter-Directed Thrombolysis in SVC Syndrome
Patient Selection
Superior vena cava syndrome (SCVS) is an obstruction of blood flow through the superior vena cava. It is a medical emergency usually manifesting a malignant disease process within the thorax in at least 60% of cases [1]. It requires immediate diagnostic evaluation and therapy. SVC obstruction was originally described by William Hunter in 1757 in a patient with a “leutic” aortic aneurysm [2], and this remained the etiology in 40% of cases until the mid-1950s. With the era of antibiotics and the eradication of syphilis and tuberculosis, the etiology of SCVS was replaced largely by malignant disease. Bronchogenic carcinoma is the underlying disease process in 70% of cases; with the addition of lymphoma, malignancy accounts for the etiology in 90% of cases [1, 3].
In the United States, SVCS develops in 5-10% of patients with a right-sided malignant intrathoracic mass lesion. In 1969, Salsali and Cliffton observed SVCS in 4.2% of 4960 patients with lung cancer; 80% of the tumors inducing SVCS were of the right lung [4]. In 1987, Armstrong and Perez found SVCS in 1.9% of 952 patients with lymphoma [5].
Malignant causes of SVCS are most commonly observed in males because of the high incidence of lung cancer in this population [1]. In contrast, no sex difference is observed in cases related to benign causes [6-12]. Malignant causes of SVCS are predominantly observed in individuals aged 40-60 years [4]. If SVCS is secondary to a malignant process, patient survival correlates with the histology of the tumor [13]. Patients with signs and symptoms of laryngeal and cerebral edema have the most life-threatening manifestations of this syndrome and are in danger of sudden death. Approximately 10% of SVCS patients with a bronchogenic carcinoma and 45% of patients with lymphoma treated with radiation live at least 30 months while patients with untreated malignant SVCS survive only 30 days [13]. Since most cases are due to malignancy, nearly all patients will receive radiation. Eighty to 90% of patients are initially relieved of SVCS; however 50% of patients relapse [14]. Relapse occurs in benign disease as well; although collaterals develop, thrombosis will continue to propagate and occlude these collaterals over time.
Benign causes which can account for approximately 10% of cases include inflammatory diseases (e.g. histoplasmosis, idiopathic fibrosing mediastinitis) and iatrogenic causes such as pacemaker electrodes, AICD electrodes, or central venous lines [6-8]. SCVS may also be due to extrinsic compression of the SVC as in the case of an obstructing mediastinal tumor or thrombosis secondary to a central line or pacemaker electrode [11, 12]. Additional less frequent causes may be atrial switch operations or ventriculo-atrial shunts [9, 10]. Benign causes account for most of the cases diagnosed in individuals aged 30-40 years. Obstruction of the SVC in the pediatric age group is rare and has a different etiologic spectrum [6-12]. Survival in patients with SVCS depends on the course of the underlying disease. No mortality, per se, results directly from mild venous congestion. In benign SVCS, life expectancy is unchanged [9, 10].
Common symptoms are feeling of fullness in the head and neck in 81% of patients; dyspnea on exertion or orthopnea (72%); headache (53%); dizziness or syncope (34%); visual problems (25%); and cough (22%) [13]. Common clinical signs are head and neck swelling (97%); large chest wall collaterals (91%); facial cyanosis (56%); arm swelling (53%) and pleural effusions (6%) [13]. Headaches and syncope are from cerebral edema from venous hypertension. These symptoms herald a reduced life expectancy of about 6 weeks and demand urgent intervention [13].
Diagnosis starts with a physical exam with a particular emphasis on the head and neck area. Chest x-ray may show a hilar mass in the case of an obstructing bronchogenic carcinoma or mediastinal mass (e.g. lymphoma) or mediastinal calcification (e.g. histoplasmosis). Infused computed tomography of the head and neck and chest with a venous phase will show characteristic pictures of numerous superficially draining contrast-filled venous collaterals (Figure 1). It will allow assessment of the mediastinum and help exclude compressive masses in the case of an externally compressive hilar or anterior mass, or exclude extensive intravascular clot secondary to a pacemaker electrode. It will also help determine the patency of the jugular and subclavian veins.
Patients with SVCS secondary to intravascular thrombosis of superior mediastinal veins as well as extrinsic compression of the superior vena cava are candidates for catheter-directed thrombolysis and stent placement. A history of bleeding diatheses may be a contraindication due to the necessary use of thrombolytics.
Operative Steps
General anesthesia is utilized. Due to the patient's upper airway swelling from SVCS, airway access may be difficult, often necessitating the use of fiberoptic intubation. The patient is positioned supine with both arms placed at 90 degrees. Both arms are prepped in as well as both groins for access. Large bore IV access may be a problem secondary to the extensive upper extremity venous collaterals. Use of the SonoSite Ultrasound® (SonoSite Inc. Bothell, WA) for deep venous access of the upper extremities may be warranted. Two short 6F sheaths placed in the right and left cephalic veins (or one placed in the upper extremity and one in the groin via the common femoral vein) are necessary for access. A soft angled Glide catheter is necessary to access the great veins of the upper mediastinum down to the superior vena cava, and a soft angled Glide catheter placed into the SVC is necessary for performing the contrast venogram of the upper extremities and SVC to localize and define the extent of clot (Figures 2A and 2B).

Figure 1: Infused CT scan demonstrating extensive contrast filled superficial venous collaterals (yellow arrow) overlying the right hemithorax and a small contrast-filled "trickle" draining centrally into a clot-filled superior vena cava (blue arrow).
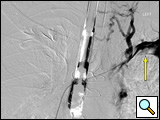
Figure 2A: AP venogram of left subclavian vein from the right groin catheter demonstrating extensive intravascular clot at the arrow and catheter tips.
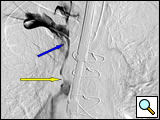
Figure 2B: Selective venogram of the right subclavian vein taken from the right brachial catheter visualizing the SVC junction with a small venous "trickle" (yellow arrow) draining into the SVC. There is extensive thrombus just at the tip of the infusion catheter and blue arrow.
The glide wire usually is advanced without difficulty through the soft clot.
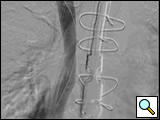
Figure 3: AP completion venogram on day 2 after mechanical thrombolysis and TPA infusion overnight and post-deployment of overlapping "kissing" Wallstents. Notice improved drainage into the right atrium on post-deployment venogram.
The Cragg-McNamara® thrombectomy catheters (MicoTherapeutics Inc, Irvine, CA) are placed and chemical thrombolysis is commenced with infusion of Alteplase® (Genetech Inc, San Francisco, CA) (dose 20 mg/100 cc normal saline) at a rate of 0.6 cc/sec through the thrombus placing it in the "power-pulse spray technique" as described by Allie et al. [15]. After allowing the TPA to sit for 20 to 30 minutes, mechanical thrombectomy is performed with the AngioJet ® rheolytic thrombectomy system (Possis Medical Inc., Minneapolis, MN) and catheter-directed thrombolysis with tissue plasminogen activator (TPA) is given overnight (2 cc/hr).
Re-imaging the following day or twelve hours later is necessary with the objective being bilateral upper extremity venograms showing a significant improvement in venous thrombosis and clot burden. Placement of two self-expanding Wallstents (Boston Scientific Inc., Natick, MA) stents centrally utilizing a "kissing stent" deployment technique [16] is warranted to avoid compression of the contralateral vessel and prevent compression of the flow channel: a 20 mm x 40 mm stent in the superior vena cava and right subclavian vein and a 14 mm x 40 mm stent in the innominate vein and superior vena cava (Figure 3). Stent sizes are selected according to patients' needs.
Preference Card
- 5F x 10 cm long micropuncture sheath w/ 21 G needle
- 19 G x 7 cm access needle
- 2 6F x 10 cm sheaths
- SonoSite® Ultrasound Probe
- Flexi tip angled Glide wire (0.035"/260 cm)
- 5F x 100 cm Aqua-Tempo® angiographic catheter (angled or straight) (Cordis Corporation-Johnson & Johnson Co., Miami Lakes, FL)
- IV contrast
- DVX 3 mm/90 cm/6F/0.038" thrombectomy catheter (Possis Medical Inc, Minneapolis, MN)
- Cragg-McNamara® (Micro Therapeutics Inc, Irvine, CA) valved infusion catheters (0.038 in/5F x 1.67 mm x 135 cm)
- AngioJet® rheolytic thrombectomy system Model 300A (Possis Medical Inc, Minneapolis, MN)
- Alteplase® (Genetech Inc. San Francisco, CA) (mixed 20 mg/100 ml normal saline)
Tips & Pitfalls
- Select patients carefully
- Adequate hydration overnight and between imaging sessions and/or the use of NaHCO3 and Mucomyst might be a consideration with elevated creatinine [17]
- Airway control and access may be an issue secondary to the swelling of the upper extremity and head and neck
- Large bore IV access may be a problem secondary to the extensive upper extremity venous collaterals and thrombosis
- Ultrasound guidance for percutaneous placement of access needles, venous sheaths, and catheters is mandatory because of the use of TPA
- Utilize standard Seldinger techniques
- Place thrombectomy catheters with the side holes lying across and through clot for adequate thrombolysis
- Employ "kissing" stent techniques for simultaneous inflation of stents
- Individualize stent sizes
Results
Historically, before the era of stenting, SVC bypass was considered with composite autogenous vein grafts or PTFE bypass grafts in benign causes or for palliation in malignant causes with severe or acute onset SVC syndrome. In a surgical series of spiral vein grafts, Doty [18] showed good durability with seven of nine grafts remaining patent for up to nearly 15 years and all but one patient being free of superior vena cava syndrome.
Currently, the treatment of patients with malignant superior vena caval obstruction with minimal morbidity has been made possible by the recent introduction of expandable metal stents as a sole palliative treatment or as an adjunct to other treatment modalities [14, 19, 20]. Surgical bypass of the SVC may be a useful way to palliate symptoms in carefully selected patients and should still be considered as a later option [7, 18]. Indications to proceed with such procedure now are much less clear; patients who are not suitable for or who fail endovascular intervention may merit open surgical reconstruction. For the most part, these are patients with advanced intrathoracic disease amenable only to palliative therapy (i.e., after failure of radiation, chemotherapy, and stent therapy).
SVC stenting can provide rapid symptomatic relief within few days in most patients with SVCS. SVC stenting may provide relief of severe symptoms for patients while the histological diagnosis of the malignancy causing the obstruction is being actively pursued. Stenting may also be indicated in patients in whom chemotherapy or radiation has failed. Some literature [13, 14, 19-23] recommends stenting as first-line treatment to be performed early in the management of SVCS. The ease of insertion with the use of local anesthesia with radiologic control, the self-expanding nature of the stent, and the lack of major complications on follow-up are particular advantages [13, 14, 19-23].
Endovascular treatment is effective over the short term; however, there is a frequent need for repeat interventions. Courtheoux and others [22], in their series of 20 patients with malignant SVCS, noted successful control in 94% of patients until death or completion of the study and in 3 patients the procedure was repeated (3 to 20 weeks later) because of the recurrence of symptoms.
Kalra and coauthors [13], in their series from Mayo only looked at the treatment of SCVS associated with benign disorders, had a significantly higher graft patency in vein grafts compared to ePTFE, with 12 secondary endovascular procedures performed to maintain patency in 11 of 12 primary surgical reconstructions.
Gross [19] showed that percutaneous implantation of Wallstent endoprostheses provides excellent palliation for SVCS. This study identified obstruction of the superior vena cava in 13 patients, who then underwent transluminal dilation and Wallstent implantation. These patients were treated with IV heparin and monitored in the emergency department. Thereafter, they were treated with a platelet inhibitor for 4 weeks. Because their signs and symptoms improved, patients were able to resume radiation therapy, chemotherapy, or both. Although eight patients died of their tumors, SVCS did not recur in any patient.
Mónaco, et al., [14], in series that had an overwhelming number of SVCS due to malignant disease, reported that all procedures were technically successful with no stent migration observed. Thirty-two patients with malignant tumors ultimately died due to progression of disease with a mean survival time of 193 days after stent placement. There was an SVCS recurrence observed on six occasions, with four patients receiving a new stent. They reported that symptomatic improvement was dramatically seen within 24–48 hours after stent placement in 40 patients (90.9%) and 83.3% out of the cases (38/44) were symptom-free during the duration of their disease.
Transcatheter thrombolytic therapy for SVCS was originally described in a 1974 report of a patient whose acute thrombosis was caused by a pacemaker lead [24]. The goal of thrombolysis in the acute setting is to dissolve the thrombus, relieve venous congestion, and restore venous return to the right atrium. Angioplasty or stent placement may then be considered to treat the underlying lesion. In an SVC that is chronically occluded and is "uncrossable" by standard guide wire and catheter techniques, catheter-directed thrombolysis initially may serve to soften or partially recanalize the vessel and eventually allow a guide wire to cross the lesion. Once the guide wire has safely traversed the obstruction, again angioplasty and stenting can dilate the occluded segment. Although many patients derive substantial benefit from thrombolysis alone, only a minority may enjoy complete relief of symptoms [23].
Kee and others [23], in their series from Stanford, looked at both catheter-directed thrombolysis and placement of stents, with an overwhelming number of patients with SVCS due to malignant disease. Among 42 patients with underlying malignancy, primary clinical patency in the malignant group was achieved in 33 (79%) and secondary clinical patency was achieved in 39 (93%). In comparison, in 13 patients with benign disease primary clinical patency was achieved in 10 (77%) and secondary clinical patency was achieved in 11 (85%).
Kishi and coauthors [21], in 11 patients with SCVS secondary to malignant disease, correlated a caval pressure of greater than 22 mmHg, lesion diameter, and symptom score to successful stent placement. Yamagami [20], employing only stenting, elegantly showed clinical improvement in edema of extremities, swelling of the face, and head and neck. They went on to quantify improvements in hemodynamic parameters such as decrease in caval pressure distal to the stenosis, which decreased in all patients experiencing a decrease of the pressure gradient across the caval lesion after stenting; increase in 24 hr urine output; and increases in right atrial pressure, pulmonary capillary wedge pressures, and cardiac outputs. This, however, was a small series of patients.
In conclusion, due to the availability of stents, the ease of their placement, and the additional supporting armamentarium of thrombolysis techniques, stent placement and catheter-directed thrombolysis may be the future paradigm in the treatment of a syndrome that is rapidly fatal if untreated. As always, the techniques listed here should be undertaken only by personnel trained in endovascular techniques. A large institutional series would be necessary to evaluate such a hypothesis.
References
- Ahmann F. A reassessment of the clinical implications of the superior vena cava syndrome. J Clin Oncol 1984;2:961-69.
- Hunter W. The history of an aneurysm of the aorta with some remarks on aneurysms in general. Med Obs Inq (Lond) 1757;1:323-57.
- Parish JM, Marschke RF Jr, Dines DE, Lee RE. Etiologic considerations in superior vena cava syndrome. Mayo Clin Proc 1981;56:407-13.
- Salsali M, Cliffton EE. Superior vena caval obstruction in carcinoma of lung. NY State J Med 1969;69:2875-80.
- Armstrong BA, Perez CA, Simpson JR, Hederman MA. Role of irradiation in the management of superior vena cava syndrome. Int J Radiat Oncol Biol Phys 1987;13:531-9.
- Chen J, Bongard F, Klein SR. A contemporary perspective on superior vena cava syndrome. Am J Surg 1990;160:207-11.
- Doty DB. Bypass of superior vena cava: Six years' experience with spiral vein graft for obstruction of superior vena cava due to benign and malignant disease. J Thorac Cardiovasc Surg 1982;83:326-38.
- Dodds GA III, Harrison JK, O'Laughlin MP, et al. Relief of superior vena cava syndrome due to fibrosing mediastinitis using the Palmaz stent. Chest 1994;106:315-18.
- Pierli C, Iadanza A, Del Pasqua A, Fineschi M. Acute superior vena cava and right atrial tamponade in an infant after open heart surgery. Int J Cardiol 2002;83:195-7.
- Stavropoulos GP, Hamilton I. Severe superior vena caval syndrome after the Mustard repair in a patient with persistent left superior vena cava. Eur J Cardiothorac Surg 1994;8:48-50.
- Kanada DJ, Jung RC, Ishihara S. Superior vena cava syndrome due to a retained central venous pressure catheter. Chest 1979;75:734-5.
- Kastner RJ, Fisher WG, Blacky AR, Bacon ME. Pacemaker-induced superior vena cava syndrome with successful treatment by balloon venoplasty. Am J Cardiol 1996;77:789-90.
- Kalra M, Gloviczki P, Andrews JC, et al. Open surgical and endovascular treatment of superior vena cava syndrome caused by nonmalignant disease. J Vasc Surg 2003;38:215-223.
- Mónaco RG, Bertoni G, Pallota G, et al. Use of self-expanding vascular endoprostheses in superior vena cava syndrome. Eur J Cardiothorac Surg 2003;24:208-11.
- Allie DE, Hebert CJ, Lirtzman MD, Wyatt CH, Keller VA, Khan MH, Barker EA, McElderry MW, Khan MA, Fail PS, Stagg SJ 3rd, Mitran EV, Chaisson G, Allie SD, Allie AA, Walker CM. Novel simultaneous combination chemical thrombolysis/rheolytic thrombectomy therapy for acute critical limb ischemia: the power-pulse spray technique. Catheter Cardiovasc Interv 2004;63:512-22.
- Mohamed F, Sarkar B, Timmons G, Mudawi A, Ashour H, Uberoi R. Outcome of "kissing stents" for aortoiliac atherosclerotic disease, including the effect on the non-diseased contralateral iliac limb. Cardiovasc Intervent Radiol 2002;25:472-5.
- Merten G, Burgess WP, Gray L, et al. Prevention of contrast-induced nephropathy with sodium bicarbonate: a randomized controlled trial. JAMA 2004;291:2328-2334.
- Doty D, Doty J, Jones K. Bypass of superior vena cava. Fifteen years' experience with spiral vein graft for obstruction of superior vena cava caused by benign disease. J Thorac Cardiovasc Surg 1990;99:889-95.
- Gross CM, Kramer J, Waigand J, et al. Stent implantation in patients with superior vena cava syndrome. AJR Am J Roentgenol 1997;169:429-32.
- Yamagami T, Nakamura T, Kato T, Iida S, Nishimura T. Hemodynamic changes after self-expandable metallic stent therapy for vena cava syndrome. Am J Roentgenol 2002;178:635-9.
- Kishi K, Sonomura T, Mitsuzane K, et al. Self-expandable metallic stent therapy for superior vena cava syndrome: clinical observations. Radiology 1993;189:531-5.
- Courtheoux P, Alkofer B, Al Refaï M, Gervais R, Le Rochais JP, Icard P. Stent placement in superior vena cava syndrome. Ann Thorac Surg 2003;75:158-61.
- Kee S, Kinoshita L, Razavi MK, Nyman U, Semba C, Dake M. Superior vena cava syndrome: treatment with catheter-directed thrombolysis and endovascular stent placement. Radiology 1998;206:187-93.
- Williams DR, Demos NJ. Thrombosis of superior vena cava caused by pacemaker wire and managed with streptokinase. J Thorac Cardiovasc Surg 1974;68:134.





Comments